Published on: August 22, 2019 | Updated on: November 5, 2024
Knees are more fragile than people believe.
The constant burden of our weight makes these joints much more susceptible to injuries, abnormalities, and complications. These issues can become most apparent when we exacerbate the knees by kneeling.
The act of kneeling requires the intricate network of muscle, ligament, tendon, and bone to work in unison – any small disruption in the dynamics of these tissues upsets the knee and may trigger pain.
Anatomy of the Knee
The knee is a complex arrangement of soft tissues, bones, and muscles which are all extremely sensitive. If this intricate network of tissues is upset even slightly and its natural rhythm is thrown off, then complications could arise and eventually insight pain. The knee is made up of:
- Bones such as…
- The patella, more commonly referred to as the knee cap, helps extend the knee by increasing the leverage that certain tendons can exert on the lower leg.
- The femur, directly behind and above the kneecap, supports the weight of the human body allowing for the motion of the leg.
- The fibula and tibia, directly under and adjacent to the patella, help stabilize the ankle and support the muscles of the lower leg.
- Soft tissues such as…
- The medial and lateral meniscus, which are found on the top and to either side of the tibia, absorb the impact of our weight on the knees.
- The posterior and anterior cruciate ligaments, located directly behind the knee, keep the knee centered, allowing for an even distribution of weight across the meniscus and lower portions of the legs.
- The medial and lateral collateral ligaments overlap the end of the femur on either side. They connect the muscles of the upper leg to the bone of the lower leg, control the sideways motion of the knee, and brace it against unusual movement.
Although they are not technically part of the knee joint, muscles such as the hamstrings and quadriceps provide the tension needed to insight the movements knees make. Abnormalities in these muscles can cause erratic movements in the knee, damaging the soft tissues and bones in the process.
If an individual is suffering from knee pain, it is likely due to the interaction between these components, past traumas they may have suffered, or degradation of the soft tissues which cushion the components from the crushing weight of the upper body.
Problems Associated with Knee Pain When Kneeling
If you experience knee pain when kneeling, it’s annoying and affects your quality of life. For the treatment, it is essential to understand why knee pain occurs in the first place.
Here are some effects of knee pain.
Limited Mobility
Pain in any form can affect the body’s mobility, and knee pain can make moving around impossible. You feel limited in performing daily tasks like house chores, working and moving around in the office, walking, etc.
Swelling
The pain is sometimes accompanied by swelling that further reduces mobility. The knee may also become stiff, making strenuous tasks like climbing the stairs or sitting and bending difficult.
Muscle Weakness
You may also feel the muscles around the kneecap weak. This is often because the muscles have to work extra hard to support the knee joint load.
Muscles, particularly the quadriceps and hamstrings, are affected by the pain and get weaker. This can affect knee stability and increase your risk of injuries.
Pain
Of course, when any part of the body is in pain, you can’t rest or do your usual tasks. The pain will affect your mood and sleep and also cause anxiety and stress.
If it continues in the long run, it can lead to obesity, which can affect cardiovascular health.
Causes
Just as the tissues which make up the knee are varied and unique, so too are the possible underlying causes of knee pain when kneeling. Most of these issues can be traced back to one of two things, either a past injury or tissue deterioration, though these causal factors are not mutually exclusive.
Past Injuries and Knee Pain
The motion dynamics of the knee are very sensitive to change. If an individual endures some kind of trauma to their knee, these dynamics change, and knee problems begin to arise.
Examples of a past trauma include:
- Anterior cruciate ligament (ACL), posterior cruciate ligament (MCL), and medial collateral ligament (MCL) strains or tears.
- When any of the major ligaments of the knee are injured, natural stability, distribution of weight, and balance become affected.
- Bone fractures
- The kneecap is one of the most commonly injured bones in the human body. When such an injury occurs, due to the constant stress of the body’s weight, the bone will likely never make a full recovery.
- Dislocation
- When the bones in the knee slip out of place, pain can be immediate. Once a dislocation occurs, the likelihood of another one increases, causing more and more pain as an individual ages.
After these traumas take place, they may be accompanied by pain due to the new biodynamics within the knee. Nerves may be pinched, bone can begin to rub against bone, and muscles can swell and become inflamed.
Tissue Deterioration and Knee Pain
Deteriorated tissue is one of the most common causes of knee pain when kneeling. As the soft tissues in the knee degrade, so do their cushioning effects.
This lack of cushion can cause many problems which ultimately cause us to feel pain as we exert force on the knee.
Some of the most common problems with tissue deterioration in the knee are:
- Osteoarthritis
- Osteoarthritis of the knee is a common condition, especially as we age. As we age, the cartilage in our joints wears away due to everyday movement. As the cartilage wears away the joints, especially the load-bearing joints such as the knee can become stiff, swell, and develop pain.
- Patellar tendonitis
- Characterized by inflammation of the tendon which connects the kneecap to the shin bone, patellar tendonitis is a product of repeated high-intensity stress on the knee. Patellar tendonitis most often occurs in athletes, especially those whose sport of choice involves jumping but can occur in anyone.
Signs and Symptoms
Though determining the underlying cause may be difficult, diagnosing knee pain is simple. The most common signs of knee trouble are:
- Swelling and stiffness
- Weakness
- Instability
- Redness and warmth to the touch
- Popping, cracking, or crunching noises
- An inability to fully straighten the knee
Experiencing any of these issues may be an indication that an individual’s knee pain when kneeling is something much larger, especially if these symptoms occur under minimal physical excursion. If these symptoms occur frequently and are accompanied by pain, it may be time to consult a doctor.
Diagnostic Methods
After setting up a consultation and discussing the types of knee issues you are experiencing, a physician will use various diagnostic methods to deduce the exact issue. These include, but are not limited to:
1. Physical Examination
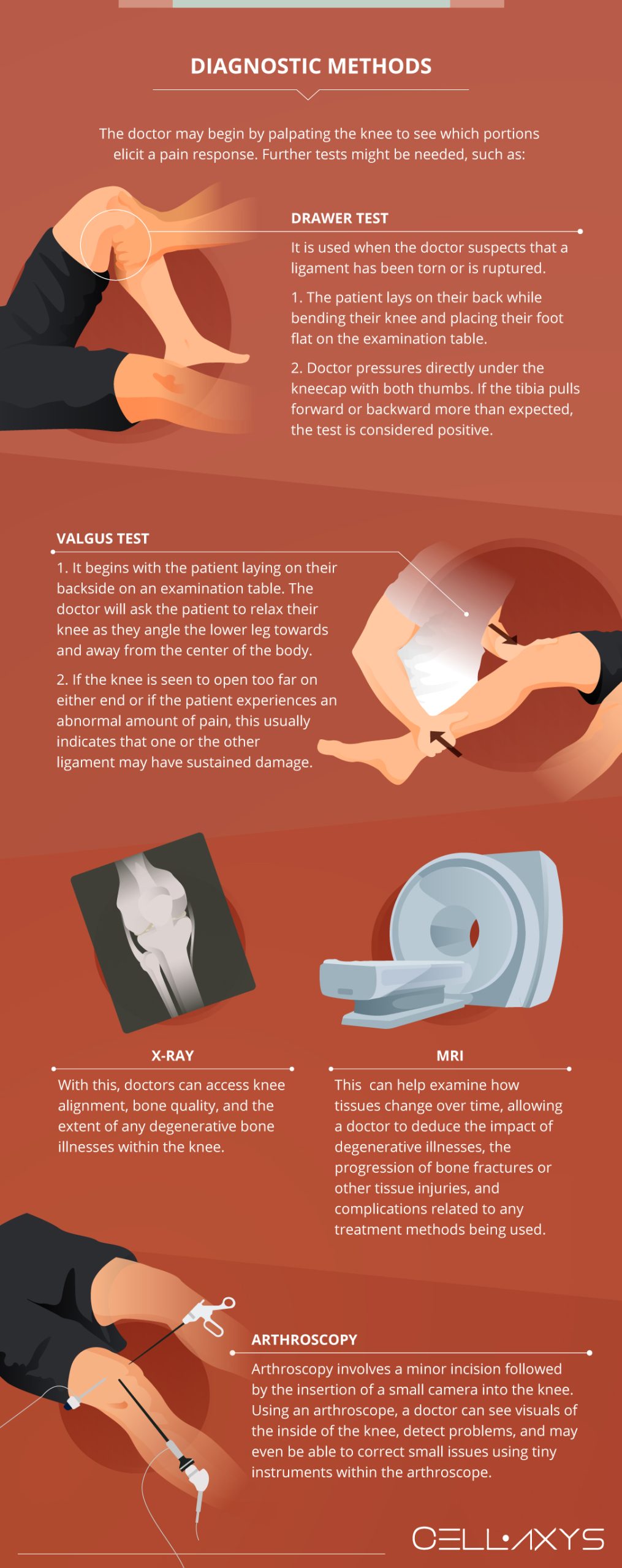
A consultation will usually lead to a physical examination of the area of pain. The doctor may begin by palpating (applying pressure to various portions) of the knee to see which portions elicit a pain response. By finding the points which provoke pain, a doctor will have a better understanding of which portions of the knee may be at risk.
2. Drawer Test
Another part of the initial clinical assessment of the knee involves what is known as a drawer test. Drawer tests are most commonly used when the doctor suspects that a ligament has been torn or is ruptured.
The patient will be asked to lay on their back while bending their knee and placing their foot flat on the examination table. By applying pressure directly under the kneecap with both thumbs, doctors can get a better idea of the state of the ligaments in the knee. If the tibia pulls forward or backward more than expected, the test is considered positive.
3. Valgus Test
Similar to the drawer test, a valgus test begins with the patient laying on their backside on an examination table. The doctor will ask the patient to relax their knee as they angle the lower leg towards and away from the center of the body.
By applying stress to the knee in this fashion, the doctor can examine the state of the MCL and LCL. If the knee is seen to open too far on either end or if the patient experiences an abnormal amount of pain, this usually indicates that one or the other ligament may have sustained some damage.
4. X-ray
X-rays give doctors a good indication of abnormalities in the structure of the bones in the knee. Using X-ray technology, doctors can access knee alignment, bone quality, and the extent of any degenerative bone illnesses within the knee. Doctors can also use X-rays to inspect past traumas and fractures, the quality of some of the soft tissues of the knee, and any abnormalities in the spaces between the major bones of the knee.
5. MRI
Magnetic resonance imaging (MRI) of the knee uses magnetic fields and radio waves to produce a detailed picture of the bones, ligaments, cartilage, tendons, muscles, and blood vessels of the knee from different angles. By examining these structures and how they change over time, a doctor can deduce the impact of degenerative illnesses, the progression of bone fractures or other tissue injuries, and complications related to any treatment methods being used.
6. Arthroscopy
A non-invasive method of looking inside the body, arthroscopy involves a minor incision followed by the insertion of a small camera into the knee. Using an arthroscope, a doctor can see visuals of the inside of the knee, detect problems, and may even be able to correct small issues using tiny instruments within the arthroscope.
A doctor may choose to use one or more of these techniques to investigate the underlying causes of your knee pain. Once they’ve found the root issue or issues, they will develop a treatment plan catered to the patient’s specific needs.
Some patients may be under time constraints, others care more about reducing pain, and some have minimal functional goals they’d like to reach. Whatever the case may be, doctors have a variety of tools at their disposal to create a treatment plan which suits the needs of their patients.
How to Manage Knee Pain
Specific lifestyle changes can significantly improve knee pain and help you go about life as usual.
Weight Management
Maintain a healthy body weight (just keep it within your BMI). This will reduce the extra strain on the knee and other muscles. You will also feel strong enough to move about by yourself and get a lot done around the house and your office.
Eat Healthy
A well-balanced diet can make a marked difference in maintaining a healthy weight and overall health. Incorporate healthy food options like lean proteins, whole foods, fruits, and vegetables into your diet.
Low Impact Exercises
Work out daily, but do some low-impact exercises. These will strengthen the muscles around the knee so they can take on the extra load and build strength. Exercises like cycling, swimming, pilates, and yoga are all recommended to build muscle strength and balance the body.
Protect the Knee
Wear a brace or knee pads to prevent falling and injuring your knee. This will also reduce the pressure on the knee and keep the pain within manageable limits.
Orthotics Footwear
Wear the right shoes or customized orthotics for better support and shock absorption.
Conventional Treatments
There is a wide variety of conventional treatment methods to help a patient reach their functional goals if they are experiencing knee pain when kneeling. Conventional treatment options are the most recommended and widely studied methods. Below are some of the most popular methods doctors will try.
RICE Therapy
Some knee issues may be as simple to treat as rest, ice, compress, and elevate. The RICE method is typically recommended at the onset of treatment due to its simplicity, though it may often be recommended during flare-ups to ease the pain and reduce the swelling an individual may experience.
Medication
Medication is an immediate solution to the pain an individual may experience due to their knee issues. While this form of treatment doesn’t solve the underlying causes of knee pain, it does provide immediate relief to the issue. If the pain is a minimal disturbance, doctors will typically recommend over-the-counter pain relievers such as acetaminophen, ibuprofen, and naproxen.
If the pain is debilitating, doctors can prescribe a stronger medication, though these come with risks. Stronger medications can become addicting, may degenerate tissue further, and their effects are known to wane over time, leading to stronger and stronger dosages and the potential risk of liver damage.
Physical Therapy
Another popular treatment option is physical therapy. Physical therapy helps individuals restructure their body’s biomechanics. By emphasizing the use of lateral muscles and boosting their strength, physical trainers can help reduce the pain an individual feels throughout their everyday motions.
Steroid Injections
There are a host of steroids that a doctor may recommend for treatment. These injections act quickly by reducing inflammation and as a result the pain an individual may feel. While steroid injections aren’t the first option for treatment, they are still popular among some of the most popular treatment methods throughout the United States.
Steroid injections have been shown to degenerate tissues further, thus increasing the magnitude of the pain an individual may feel. Over time, steroid injections run the risk of causing debilitating pain and even permanent damage to the area they are meant to treat.
Surgery
Surgery is often the last resort for individuals seeking pain relief. Long recovery periods, expensive medical bills, and variable success rates make surgery an impractical solution for knee pain treatment.
Regenerative Therapies
Recent advancements in regenerative sciences have popularized orthobiologic treatments across the globe. These include platelet-rich plasma (PRP) and cell-based therapies.
Both of these therapies work similarly. Doctors extract tissues directly from the patient’s body, process them, and then reinject them into the injury site. These cells then create a suitable environment for tissue repair by calling the body’s natural healing factors to the site of injury.
- Platelet-Rich Plasma (PRP) Therapy. The PRP procedure isolates platelets from the patient’s blood plasma and then injects them into the injured knee. Platelets are healing components of our body that release 10 Growth Factors to promote the growth of healthy tissues. They also send chemical signals to attract healing cells in your blood and creates a web-like sticky structure called fibrin. This speeds up the recovery at the injury site.
- Cell-Based Therapies. Also known as stem cell therapies, cell-based therapies involve harvesting healthy cells from your adipose (fat) tissue called Minimally Manipulated Adipose Tissue (MMAT) transplant or bone marrow called Bone Marrow Concentrate (BMAC) and reinjecting them into your injury site.
PRP therapies take about 45 minutes to complete, while both types of cell-based therapies are completed in 1.5 to 2 hours. PRP and cell-based therapies are outpatient procedures, which means you can go home right after the procedure.
Orthobiologic treatment methods are being widely studied and have become more accepted as an alternative treatment to not only joint issues, but soft tissue, muscle, and even bone damage.
Sources
Footnotes
- Atukorala I, Pathmeswaran A, Chaturanga Y, Chang T, Zhang Y, Hunter DJ. Is knee buckling, knee injury, squatting and kneeling associated with pain flares in knee osteoarthritis?. Osteoarthritis and Cartilage. 2021;29:S230.
- Wylde V, Artz N, Howells N, Blom AW. Kneeling ability after total knee replacement. EFORT open reviews. 2019;4(7):460-7.
- Centeno CJ, Pastoriza SM. Past, current and future interventional orthobiologics techniques and how they relate to regenerative rehabilitation: a clinical commentary. International Journal of Sports Physical Therapy. 2020;15(2):301.
- Welton KL, Logterman S, Bartley JH, Vidal AF, McCarty EC. Knee cartilage repair and restoration: common problems and solutions. Clinics in sports medicine. 2018;37(2):307-30.
- Pountos I, Panteli M, Walters G, Bush D, Giannoudis PV. Safety of epidural corticosteroid injections. Drugs in R&D. 2016;16:19-34.
- DeChellis DM, Cortazzo MH. Regenerative medicine in the field of pain medicine: Prolotherapy, platelet-rich plasma therapy, and stem cell therapy—Theory and evidence. Techniques in Regional Anesthesia and Pain Management. 2011;15(2):74-80.
References
- What to know about knee pain when kneeling. Medical News Today. Accessed 2/26/2024.
- Knee Pain Kneeling. Knee Pain Explained. Accessed 2/26/2024.
- Kneeling Pain: What can I do about it?. Core Concepts. Accessed 2/26/2024.
CELLAXYS does not offer Stem Cell Therapy as a cure for any medical condition. No statements or treatments presented by Cellaxys have been evaluated or approved by the Food and Drug Administration (FDA). This site contains no medical advice. All statements and opinions are provided for educational and informational purposes only.
Dr Pejman Bady
Author
Dr. Pejman Bady began his career over 20 years ago in Family/Emergency Medicine, working in fast-paced emergency departments in Nevada and Kansas. He has served the people of Las Vegas as a physician for over two decades. Throughout this time, he has been met with much acclaim and is now the head of Emergency Medical Services in Nye County, Nevada. More about the doctor on this page.
Dr Pouya Mohajer
Contributor
Pouya Mohajer, M.D. is the Director of Spine and Interventional Medicine for CELLAXYS: Age, Regenerative, and Interventional Medicine Centers. He has over 20 years of experience in pain management, perioperative medicine, and anesthesiology. Dr. Mohajer founded and is the Medical Director of Southern Nevada Pain Specialists and PRIMMED Clinics. He has dedicated his career to surgical innovation and scientific advancement. More about the doctor on this page.