Published on: August 29, 2022 | Updated on: August 29, 2024
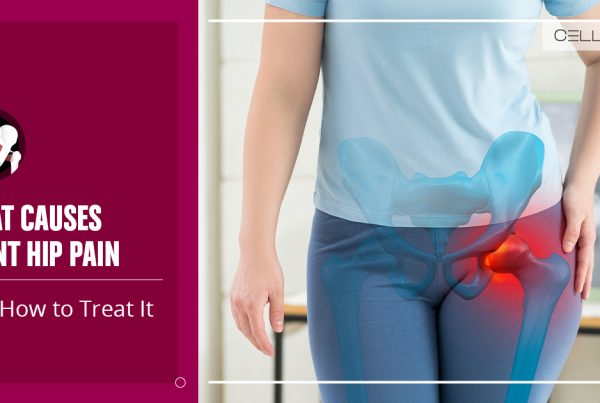
Hip replacement surgery can be a very safe and successful procedure to repair severe damage to the hips and joints. With a success rate of over 90%, it is considered one of the best-performing procedures in modern medicine and leads in terms of positive outcomes. However, even the most successful hip replacement is not immune to postoperative aches and pains, the most common of which are pains in or around the buttocks.
The pain does not render you immobile and does not indicate an unsuccessful surgery, as it is entirely normal following a hip replacement. But what exactly causes it? Since the procedure is meant to repair that region or part, why do the surrounding areas ache afterward? It may not indicate other complications (the opposite), but it is nonetheless uncomfortable and may create some complications along the recovery process.
With that in mind, we can examine exactly what these pains are and how to relieve them to make your 2-3 month recovery as smooth as possible.
The Connection of Hips to Buttocks
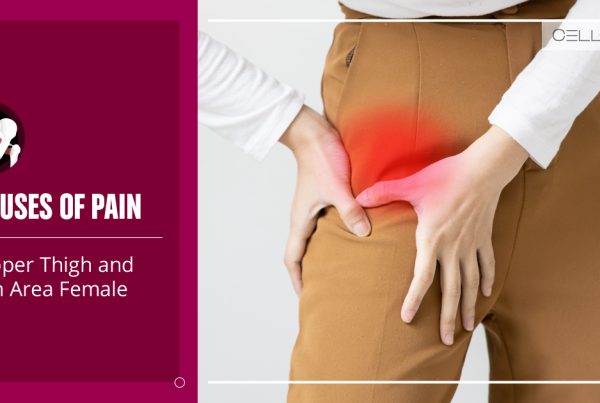
Anatomically, the buttocks and hips are interconnected through the pelvis and a series of muscles. One muscle in particular, the piriformis muscle, is a muscle in the buttocks that connects to just above the hip joint. So, when the hip undergoes surgery, we feel it in those surrounding areas.
The perfect example would be in the actual gluteal muscles. Your maximum, minimus, and medius also act as the protectors of the hip joints, so they are directly connected when you get the hip replacement. The hip joint may have been improved, but it can leave the issue of affecting these gluteal muscles and causing gluteal tendinopathy. Platelet-rich plasma or PRP therapy is the most common way to treat tendon issues, but an MRI scan will pinpoint precisely where you have these issues as well as their level of potential damage.
Common Post-Hip Replacement Pains
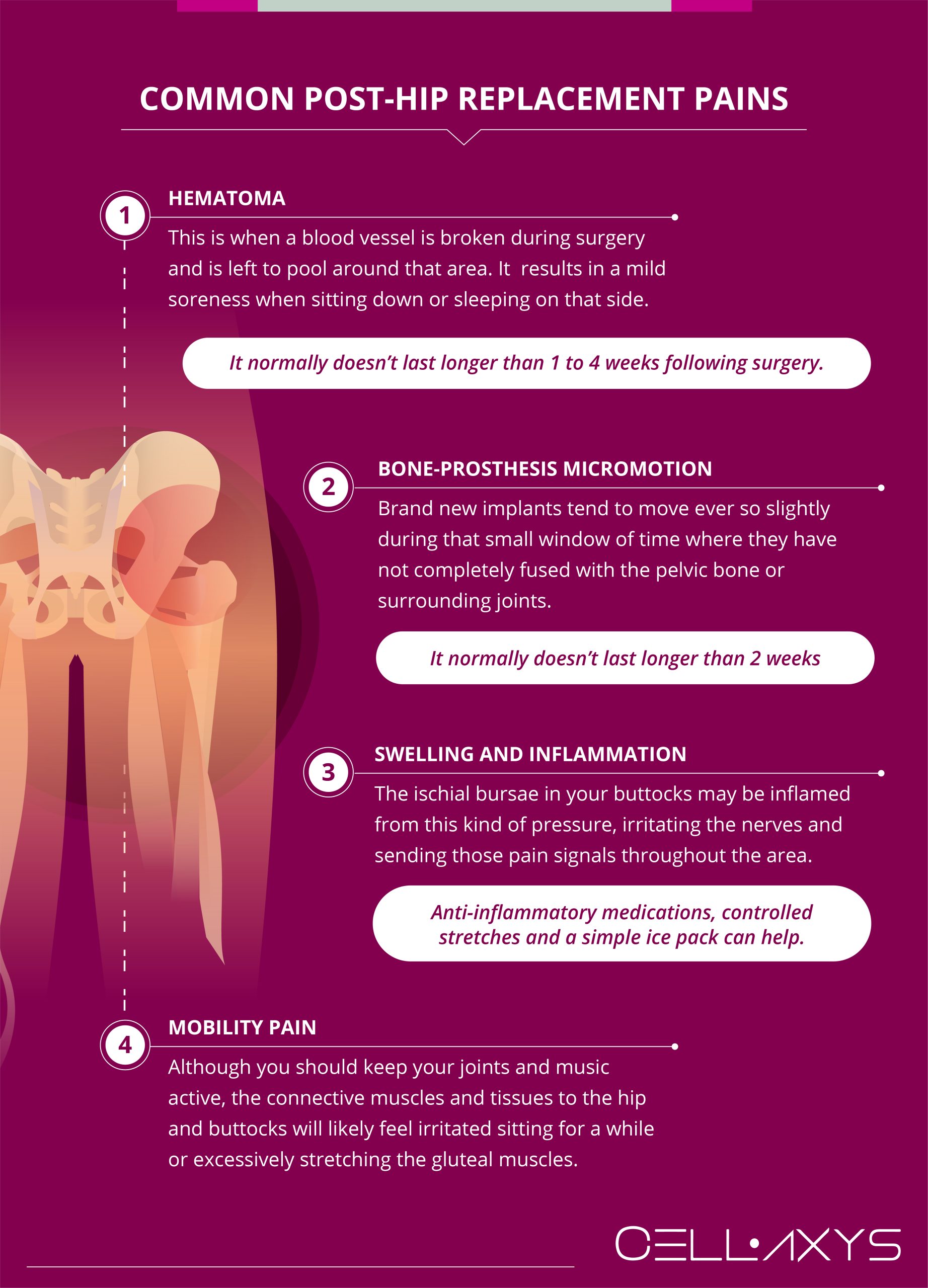
Again, the pelvis and surrounding regions of the hip are affected by the surgery, making it completely normal to experience discomfort in the buttocks, groin, and thighs. This does not create several complications, and most likely do not need surgery, but it is beneficial to how they affect you and how they can be treated.
Hematoma
Hematoma is most common after a THR (or a total hip replacement) or hip arthroplasty (THA) despite only being reported in about 2% of patients. This is when a blood vessel, basically internal bleeding, is broken during surgery and is left to pool around that area. What hematoma creates is similar to a bruise from the blood pooling under the skin, making that area slightly discolored and lumpy.
During the surgery, there is a chance that a blood vessel in the gluteal muscles could have been damaged along the way, resulting in mild soreness when sitting down or sleeping on that side.
Since it is merely blood pooling to one spot, this is usually resolved by letting the excess blood spread evenly and smooth out naturally. It generally takes no longer than 1 to 4 weeks following the surgery. The only time a hematoma is of concern for further attention is when it grows over time instead of receding or is visible after four weeks to 2 months.
Bone-Prosthesis Micromotion
For your surgery to be successful and for your new implant to stay in place so it can function adequately, the implant needs to be stable and cemented. However, brand-new implants move slightly when not completely fused with the pelvic bone or surrounding joints.
If you have ever experienced degenerative disc joints, the bones in your spine start to rub together when they are not supposed to, leading to significant discomfort. Following a hip replacement, you may feel a similar pain in the thigh and buttocks in the first few weeks of your recovery. 2 weeks of this is standard, but it can lead to implant failure if it is not treated correctly.
Swelling and Inflammation
Much like the hematoma, it is expected to experience inflammation and swelling in or around the surgical wound, buttocks, or the areas that are applied the most pressure. Specifically, the ischial bursae in your buttocks may be inflamed from this pressure, irritating the nerves and sending pain signals throughout the area.
Quite possibly the easiest of these pains to treat, a semi-regular dose of ibuprofen or other anti-inflammatory medications should do just the trick. After a hip replacement, too much mobility may seem like it would be harmful (which it is), but controlled stretches for only a few minutes will also ease the pain and strengthen the muscles and tendons, while a simple ice pack can still accelerate the healing from inflammation.
Mobility Pain
Lastly, as much as it is necessary to take care of your joints and muscles by keeping them active, this understandably becomes difficult for about one-month post-operation. The connective muscles and tissues to the hip and buttocks will likely feel irritated sitting for a while or excessively stretching the gluteal muscles.
Your body is still adjusting itself to work with the implant, so those first few weeks are when the pain is most noticeable. But all is not lost: Resting your body is still a viable option when you are not in physical therapy, and you can return to doing what you love early in your recovery.
Is Buttock Pain Normal After Hip Surgery?
As mentioned earlier, your gluteal muscles protecting the hip joints are in the direct path of your hip replacement surgery, so it is normal for them to feel tender or sore following the operation. It is considered part of the healing process, typically lasting about three months. If your operation was not for both hips, then the side opposite of your incisions will not feel nearly as sore, but it can feel like an inconvenience to have one side sorer than the other.
When Should I Go Back to the Doctor?
Leading up to your hip replacement, you were likely aware of what kind of complications you had in that area, as well as the severity of the pain. You will know that if the discomfort in the buttocks or the pelvic region is worse than that of a sprain, then it would be an ideal time to take medications. It is time to revisit the doctor if it is worse than that (hopefully not).
What Relieves The Pain?
It may initially sound complicated, but keep moving to relieve the pain. A walk around the block a couple of times a day for a few weeks, followed by an ice pack on the inflamed areas, will keep those muscles strong, stress-free, and active, which subdues the pain.
Sources
Footnotes
- Uchida S, Kizaki K, Hirano F, Martin HD, Sakai A. Postoperative Deep Gluteal Syndrome After Hip Arthroscopic Surgery. Orthopaedic Journal of Sports Medicine. 2020;8(9).
- Lesher JM, Dreyfuss P, Hager N, Kaplan M, Furman M. Hip joint pain referral patterns: a descriptive study. Pain Medicine. 2008;9(1):22-5.
- Berge DJ, Dolin SJ, Williams AC, Harman R. Pre-operative and post-operative effect of a pain management programme prior to total hip replacement: a randomized controlled trial. Pain. 2004;110(1-2):33-9.
- Mortazavi SJ, Hansen P, Zmistowski B, Kane PW, Restrepo C, Parvizi J. Hematoma following primary total hip arthroplasty: a grave complication. The Journal of arthroplasty. 2013;28(3):498-503.
- Pipino F. The bone-prosthesis interaction. Journal of Orthopaedics and Traumatology. 2000;1:3-9.
References
- Hip Replacement. HSS. Accessed 9/6/2023.
- Painful hip arthroplasty: definition. NIH. Accessed 9/6/2023.
- The painful total hip replacement. The Bone & Joint Journal. Accessed 9/6/2023.
CELLAXYS does not offer Stem Cell Therapy as a cure for any medical condition. No statements or treatments presented by Cellaxys have been evaluated or approved by the Food and Drug Administration (FDA). This site contains no medical advice. All statements and opinions are provided for educational and informational purposes only.
Dr Pouya Mohajer
Author
Pouya Mohajer, M.D. is the Director of Spine and Interventional Medicine for CELLAXYS: Age, Regenerative, and Interventional Medicine Centers. He has over 20 years of experience in pain management, perioperative medicine, and anesthesiology. Dr. Mohajer founded and is the Medical Director of Southern Nevada Pain Specialists and PRIMMED Clinics. He has dedicated his career to surgical innovation and scientific advancement. More about the doctor on this page.
Dr Pejman Bady
Contributor
Dr. Pejman Bady began his career over 20 years ago in Family/Emergency Medicine, working in fast-paced emergency departments in Nevada and Kansas. He has served the people of Las Vegas as a physician for over two decades. Throughout this time, he has been met with much acclaim and is now the head of Emergency Medical Services in Nye County, Nevada. More about the doctor on this page.