Published on: December 6, 2019 | Updated on: August 29, 2024
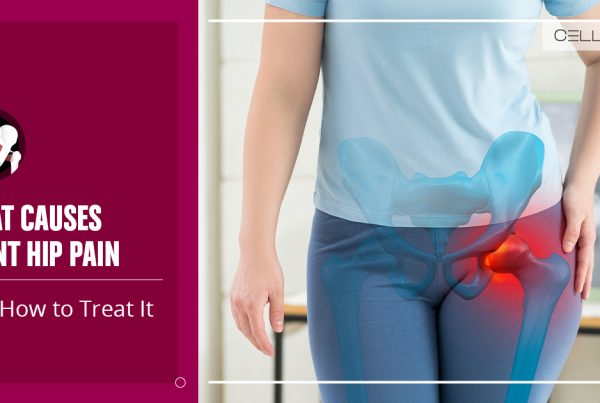
Hip replacement surgery, also known as total hip arthroplasty, may be an option for you if your hip discomfort is interfering with your everyday activities and nonsurgical therapies haven’t helped or are no longer effective.
The time it takes to recuperate from a hip replacement varies from person to person. The majority of patients can walk with help the day of or the day following surgery. After hip surgery, they normally return to normal activities between 10 and 12 weeks. The recuperation time after a full hip replacement is 6 to 12 months, although the implants can last up to 20 years.
Anatomy of the Hip
As the meeting point between the lower and upper body, the hip is largely responsible for much of the stability involved in daily movement. At this point, the thigh bone meets the pelvis and forms what is known as a ball-and-socket joint – where the rounded end of one bone nests into a smooth gap in another.
As a ball-and-socket joint, the hip is made up of two main components:
- Femoral head: the globular end of the top of the thigh bone (femur)
- Acetabulum: the “socket” portion of the hip into which the femoral head nests
These two bones are held together with bands of tissue known as ligaments which stabilize the interactions between the two components and form what is known as a joint capsule. This capsule is filled with a thin, membranous lining known as synovium which helps lubricate the joint and provide smooth interaction between the two bones.
In addition to the synovial lining, fluid-filled sacs known as bursae provide a cushion to ease the friction between the tendons, ligaments, bones, and muscles which provide the hip motions we are so used to.
Hip movement would not be possible without the muscle groups which surround the ball-and-socket joint. These muscles include:
- Gluteals: the buttocks muscles which are located at the back of the hip
- Adductor muscles: the inner thigh muscles which help to close and extend the gap between the legs
- Iliopsoas muscle: the muscle which begins at the back and forms a tight bond with the upper femur of each leg
- Quadriceps: the primary stabilizing muscles of the hip, four of them run from the hip to the knee to help provide forward movement as well as stability
- Hamstrings: the muscles at the back of the hip which run to just below the knee
With so many components acting together under extreme weight-bearing pressure, the hip is easily one of the most problematic joints in the body. The major nerves and blood vessels which run throughout the hip can easily become damaged and cause painful reactions to those who suffer hip injuries.
Additionally, the daily stress of movement can degenerate cartilage, rupture the synovial lining, or harm the bursae which can lead to major complications over time. These soft tissues provide necessary cushioning throughout the hip and as they wear away, it becomes much easier to damage the muscle and bone found throughout the hip. As these issues become aggravated, invasive treatments may be necessary.
Stages of Diagnosis for Hip Replacement
Hip replacement surgery is a highly invasive procedure; discussing alternative treatments with your doctor should be the first step you take before jumping to total hip replacement. But, when hip pain is so severe that it interferes with your daily activity, you may start to consider hip replacement as the only worthwhile option.
Hip replacement only really becomes an option after less invasive approaches have been attempted thoroughly. Once medication, physical therapy, and the use of a walking aid no longer provide enough relief from hip pain, surgical intervention will become the next thing doctors recommend.
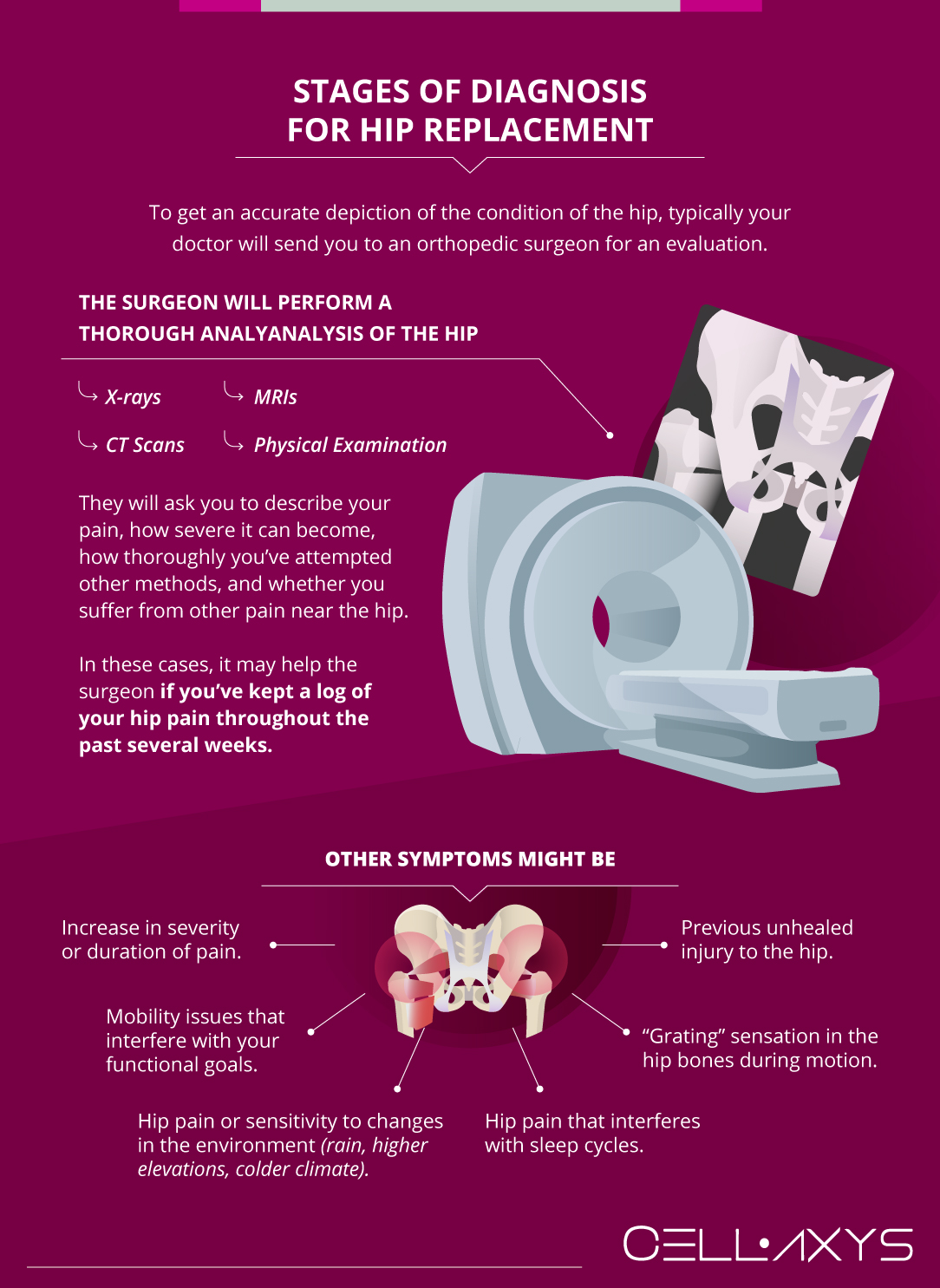
To get an accurate depiction of the condition of the hip and whether a hip replacement would be suitable, typically your doctor will send you to an orthopedic surgeon for an evaluation.
The surgeon will perform a thorough analysis of the hip by analyzing X-rays, CT scans, and MRIs after a physical examination. They will ask you to describe your pain, how severe it can become, how thoroughly you’ve attempted other methods, and whether you suffer from other pain near the hip. In these cases, it may help the surgeon if you’ve kept a log of your hip pain throughout the past several weeks.
If X-rays show structural changes within the hip, surgeons may recommend a hip replacement. If MRIs have detected early signs of degenerative illness, this may also indicate it is time for a replacement.
Other signs and symptoms that it may be time to replace your hip include:
- Increase in severity or duration of pain
- Mobility issues that interfere with your functional goals
- Hip pain or sensitivity due to changes in the environment – rain, higher elevations, colder climate
- Hip pain that interferes with sleep cycles
- “Grating” sensation experienced in the bones of the hip during motion
- Previous injury to the hip which did not heal properly
Making the Decision
For major surgeries such as hip replacement the decision ultimately falls on the patient. It is up to you to decide whether you are ready to deal with the lifestyle changes that hip replacement surgery would involve and the possible consequences the surgery may have afterward.
Financial status, age, the success rate of surgery, and possible side effects should all be taken into account before deciding to opt for hip replacement.
Once the decision has been made, there are several preparatory steps a person should take before surgery. It is best to talk to your doctor about what surgery will look like before, during, and after and discuss each possible scenario thoroughly with loved ones before proceeding.
Hip Replacement Surgery Timeline
The trajectory a particular hip replacement surgery takes varies with each patient. The following is a brief overview of some of the critical points in time for a typical hip replacement surgery, and though these may not reflect your exact procedure, they will give you a good idea of what you can expect.
- Preparing for hip replacement surgery: Successful surgeries begin with adequate preparation. These preliminary steps help ensure patient safety and may be critical in determining the outcome of the hip replacement.
- A patient should schedule blood work to mitigate outside risk factors, arrange for rides to and from the hospital, request time off work, and prepare a small parcel of luggage to last through the days after surgery.
- Follow your doctor’s instructions precisely. If they give a timeline to refrain from eating or drinking, it is important to follow these guidelines as anesthetics may interfere with the body’s natural digestive processes leading to complications during surgery.
- Maintaining an adequate sleep schedule can help boost the body’s resilience to post-surgical pain and may amplify its healing processes as well.
- Ask your doctor about the anesthetic being used. Patients may find that the type of anesthetic administered interferes with a previously undisclosed ailment.
- You may need to donate some of your blood in the weeks leading up to surgery as hip replacement may require a blood transfusion. Consult your doctor to see if this may be an option.
- Once all preparatory steps are complete, make sure to check into the hospital in a timely manner to ensure doctors have enough time to go through their pre-surgical procedures.
- The procedure: Hip replacement typically takes several hours. Once the surgery is finished, doctors will monitor the patient as they come off anesthesia before moving them to their hospital room.
- Whether you opted for traditional or minimally invasive surgery, each procedure will begin with the application of an anesthetic to relax the muscles and put you into a deep sleep.
- While you are unconscious, the surgeon will make an incision along the side of the hip, moving the muscles connected to the top of the femur to expose the hip joint.
- With the hip exposed, the femoral head is removed with a saw and an artificial one is grafted on using special cement-like material to ensure it holds.
- The socket of the hip joint is then cleaned to remove damaged cartilage and synovial lining and the artificial femoral head is inserted back into the cleaned socket. Doctors may insert a drain to ensure excess fluid can exit.
- Finally, the doctor re-attaches the moved muscle and closes the incision.
- Next, the doctor cleans the surface of the hipbone and connects the replacement socket to the hipbone, eliminating any damaged cartilage. After that, the replacement ball portion of the thighbone is put into the hip socket. A drain may be inserted to assist in the drainage of any fluid. The muscles are then reattached and the wound is closed.
- If there has been substantial blood loss, doctors may perform a blood transfusion in order to ensure patient stability and health.
- First few hours after surgery: Anesthesia will be applied routinely throughout the first few hours after the surgery. Doctors will monitor vital signs to ensure the surgery was successful and check that excess fluid is withdrawing properly from the drain which may have been placed during surgery.
- 1-2 days after surgery: Recovery for hip replacement surgery is typically short. While regular functionality isn’t immediate, patients will be asked to move within 1-2 days after surgery.
- A physical therapist will be assigned to you and begin a routine of light exercise to ensure the new hip “takes”.
- Moving to the edges of the bed, assisted standing, and walking may be attempted during these sessions immediately following surgery.
- In some cases, patients may be asked to perform these light tasks on the same day of their surgery.
- 1-week after operation: Patient activity levels will gradually be increased and the patient will be released upon approval by the physical therapist.
- Once the patient is home, they will be asked to follow the exercise routines their physical therapist taught them as well as apply any medication the doctors have prescribed.
- Creams, ointments, and oral medication should be taken as doctors have prescribed and activity levels should be moderate.
- Simple physical therapy such as massage and hot/cold treatments can be applied if medication and rest do not help alleviate post-surgical pain. Consult a doctor if you experience excruciating pain or if you suffer a hip injury immediately following replacement surgery.
- 1-month after operation: Light activities can resume and physical therapy may intensify.
- At this point, the surgical wounds have still not fully healed, but normal activity levels should resume, albeit with minimal pain and discomfort.
- Extended use may cause flare-ups of pain, but these bouts of pain should wane over time until the wounds fully recover.
- 1-year after operation: By this time the pain from surgery should be gone, and normal activity levels should return. While pain and discomfort may be inevitable, these pains should not be so excruciating that they prevent functionality.
Hip Replacement Recovery and Regenerative Medicine
Hip replacement surgeries are typically very successful, though the recovery process can be time-consuming and highly invasive. Between routines of medication and physical therapy as well as the mundanity of low activity levels, many people prefer regenerative therapies to boost the body’s natural healing processes to speed recovery after hip replacement surgery.
Regenerative therapies such as Cell-Based Therapies, or “autologous stem cells transplants,” and platelet-rich plasma (PRP) include injections of processed adult tissue such as blood, adipose (fat), and bone marrow that are meant to create an environment suitable for the repair of damaged tissue.
By isolating the platelets in the blood, PRP therapies use the platelet’s natural release of chemical impulses to draw fresh tissues to the site of an injury. Additionally, these platelets latch onto the injury and use these fresh tissues to help reduce post-surgical symptoms such as inflammation and stiffness.
Cell Base Therapies, using autologous stem cells,work much the same way. Extracting adipose or bone marrow from a patient and processing these tissues in such a way to concentrate the stem cells and healing cells and then transplanting them into the affected hip can help boost a patient’s healing responses. Once inside the body, these stem cells help to nourish the surrounding tissues.
By using these therapies in unison, many patients have found relief from post-surgical symptoms and found that their recovery processes take much less time.
If you would like to learn more about how regenerative therapies can help you recover from hip replacement surgery more quickly, contact the CELLAXYS offices today to set up a consultation.
Sources
Footnotes
- Ibrahim MS, Twaij H, Giebaly DE, Nizam I, Haddad FS. Enhanced recovery in total hip replacement: a clinical review. The bone & joint journal. 2013;95(12):1587-94.
- Biau DJ, Porcher R, Roren A, Babinet A, Rosencher N, Chevret S, Poiraudeau S, Anract P. Neither pre-operative education or a minimally invasive procedure have any influence on the recovery time after total hip replacement. International orthopaedics. 2015;39:1475-81.
- Browne JP, Bastaki H, Dawson J. What is the optimal time point to assess patient-reported recovery after hip and knee replacement? A systematic review and analysis of routinely reported outcome data from the English patient-reported outcome measures programme. Health and quality of life outcomes. 2013;11(1):1-7.
- Grant S, St John W, Patterson E. Recovery from total hip replacement surgery:“it’s not just physical”. Qualitative Health Research. 2009;19(11):1612-20.
- Naylor JM, Harmer AR, Heard RC, Harris IA. Patterns of recovery following knee and hip replacement in an Australian cohort. Australian Health Review. 2009;33(1):124-35.
- Finan PH, Goodin BR, Smith MT. The association of sleep and pain: an update and a path forward. The journal of pain. 2013;14(12):1539-52.
References
- Hip Replacement Recovery: Q&A with a Hip Specialist. Johns Hopkins Medicine. Accessed 2/23/2024.
- Hip Replacement Recovery. NHS. Accessed 2/23/2024.
- Hip Replacement. HSS. Accessed 2/23/2024.
- A Patient’s Guide to Total Hip Replacement Recovery. HSS. Accessed 2/23/2024.
- Slideshow: Hip Surgery Recovery Timeline. WebMD. Accessed 2/23/2024.
CELLAXYS does not offer Stem Cell Therapy as a cure for any medical condition. No statements or treatments presented by Cellaxys have been evaluated or approved by the Food and Drug Administration (FDA). This site contains no medical advice. All statements and opinions are provided for educational and informational purposes only.
Dr Pouya Mohajer
Author
Pouya Mohajer, M.D. is the Director of Spine and Interventional Medicine for CELLAXYS: Age, Regenerative, and Interventional Medicine Centers. He has over 20 years of experience in pain management, perioperative medicine, and anesthesiology. Dr. Mohajer founded and is the Medical Director of Southern Nevada Pain Specialists and PRIMMED Clinics. He has dedicated his career to surgical innovation and scientific advancement. More about the doctor on this page.
Dr Pejman Bady
Contributor
Dr. Pejman Bady began his career over 20 years ago in Family/Emergency Medicine, working in fast-paced emergency departments in Nevada and Kansas. He has served the people of Las Vegas as a physician for over two decades. Throughout this time, he has been met with much acclaim and is now the head of Emergency Medical Services in Nye County, Nevada. More about the doctor on this page.