Published on: July 8, 2019 | Updated on: November 5, 2024
Table of contents
- Intro
- Dangers of Running
- Running Risks for the Heart
- How Jogging Affects Your Heart
- Jogging Injuries: Runner’s Knee
- What Causes Runner’s Knee
- Conventional Treatments for Runner’s Knee
- Can Surgery Be an Effective Treatment for Runner’s Knee?
- How to Prevent Injury for Joggers?
- Regenerative Treatments for Jogging Injuries
When done smartly and with precautions, running can be one of the most rewarding exercises one can partake in. However, there are serious dangers in jogging—both to your cardiovascular system and lower legs.
Like many things in life, running can be a blessing and a curse. With proper form and pacing, running can be a renewable source of fulfillment; when done improperly, running can be detrimental — in extreme cases, even fatal.
The Copenhagen City Heart Study has shown that the fastest, most frequent runners are more likely to die prematurely from jogging than their sedentary, non-jogging counterparts.
Running is dangerous because it is prolonged and repetitive, which makes even tiny errors serious in the long run. You might lift a weight far beyond your normal range once and not get an injury, but run with an improper form for 30 minutes a day, 200 days a year, and your body will eventually break down.
How can running be dangerous for your heart? How to prevent jogging injuries? Find out all that and much more here!
Dangers of Running
Although running is an amazing sport with many cardiovascular benefits, it has a downside, too.
Running can improve blood circulation, reduce blood pressure, and improve health. However, if overdone without precaution, especially in those with underlying health conditions, it can negatively affect the heart.
As you run, the heart works harder and harder to pump blood through the body. This increases strain on the heart muscle, which has to pump harder to ensure a supply all over the body.
This actually strengthens the heart muscles and improves cardiovascular strength. But if you push too hard, you may put too much strain on the heart. This could lead to heart injury or excessive strain.
Running Risks for the Heart
Running poses severe risks for the heart:
- Sudden Cardiac Arrest: Although it’s not very common, intense running can cause a heart attack or arrhythmias in those people with undiagnosed heart conditions in marathons and high endurance races.
- Atrial Fibrillation (AFib): You may develop AFib in the long run, a condition in which the heart beats irregularly and rapidly due to overstimulation. This increases the risks of stroke and heart failure over time.
- Inflammation: Overexerting yourself, like when running when you have infections, can cause myocarditis, a condition in which the heart muscles become weak. This can cause long-term complications for the heart.
How Jogging Affects Your Heart
Sweat and hot temperature are no news to an experienced runner. Many runners appreciate the feeling. However, failing to manage your temperature can hurt your heart.
Hypothermia is a condition when your body loses heat faster than it generates it. This can lead your body temperature to drop low enough to interfere with your heart’s function. In extreme cases — or when chronically untreated — hypothermia can cause a complete failure of your heart.
Your body has self-regulatory mechanisms (sweating, breathing) that try to keep us alive and healthy in all situations. However, when you suddenly change the variables (start running after a long break, run in different conditions, try a new program), these mechanisms can turn against us.
In running — given you don’t have a related medical condition — hypothermia mostly occurs due to excessive sweating, which happens when:
- You put on excessive clothing, especially when running in cold weather.
- You run in the sun.
- You push your pace to the extremes.
Another risk factor is running in strong wind. Strong blows of wind can drastically reduce the temperature of your body.
Hypothermia also is more likely to occur in people of older age or when you’re exhausted.
How to Avoid Hypothermia?
Here’s how you can avoid hypothermia:
- Don’t run in extremely cold, hot, or windy conditions.
- If running in cold weather, make sure your outfit contains heat and includes layers of moist absorbing clothing.
- Run in the woods, where there’s a lot of shade.
- Approach running gradually. If you feel symptoms of hypothermia (shivering, low energy, slurred speech), take it down a notch.
Jogging Injuries: Runner’s Knee
Running is a non-stop shock for your bones and joints. So, if you do decide to go for a jog, it’s in your best interests to at least do it correctly. Studies estimate that up to 80% of runners experience injuries such as patellofemoral pain syndrome (better known as the runner’s knee), shin splints, and stress fractures.
Patellofemoral pain syndrome is not exactly a condition, but rather a collection of symptoms associated with several potential conditions in the knee area. It is reported that up to 25-30% of all injuries observed in sports medicine are related to the knees and that it accounts for 33% and 18% of all knee injuries in female and male athletes, respectively.
As the name suggests, runner’s knee is most common among frequent runners. However, patellofemoral pain syndrome can develop from several activities that put stress on the knees (such as soccer, long-distance walking/hiking, skiing, cycling, or playing tennis.)
In the most simple of terms, the syndrome occurs when your kneecap does not run smoothly up and down the trochlea—its dedicated “track.”
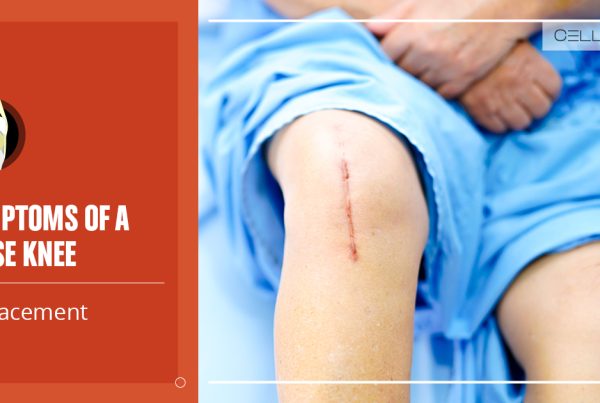
According to a Harvard Health Blog article, runner’s knee manifests as chronic, dull pain, activated by a certain motion.
The runner’s knee surfaces as dull, aching pain around or behind the kneecap. The pain is usually felt when moving (walking, jumping, running, sitting up and down.) It is not uncommon for patients diagnosed with the runner’s knee to hear popping in the knee when standing up or simply bending the knee. Sometimes, the pain is accompanied by swelling and grinding in the knee area.
What Causes Runner’s Knee
A structural problem or a certain walking or running technique might create a runner’s knee. Other factors to consider are:
- Weak thigh muscles.
- Kneecap that is excessively high in the knee joint.
- Hamstrings that are too tight.
- Achilles tendons that are too tight.
- Inadequate foot support.
- Walking or jogging with the feet inside and the kneecap pulled outward by the thigh muscles.
- Excessive training or overuse can lead to injury.
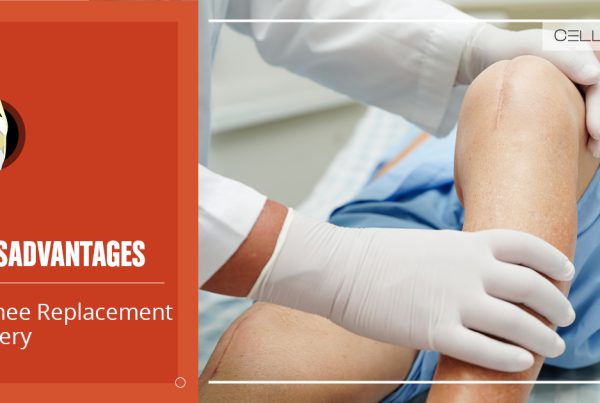
Conventional Treatments for Runner’s Knee
Due to the varying nature of the runner’s knee pain, the treatment can be very different in terms of approach and intensity. For everyday prevention, the acronym RICE represents a set of techniques that can be practiced by anyone feeling pain around their kneecaps:
- Rest: Allow for your knee joint to rest and recover.
- Ice: Apply an ice pack or a pack of frozen peas to the knee for up to 30 minutes at a time to minimize discomfort and swelling, and avoid applying heat to the knee.
- Compression: Wrap an elastic bandage or sleeve over your knee to reduce swelling, but not so tightly that it causes swelling below the knee.
- Elevation: When sitting or lying down, place a cushion beneath your knee to avoid additional swelling. Keep the foot raised above the knee and the knee lifted above the level of the heart.
Can Surgery Be an Effective Treatment for Runner’s Knee?
In short, no. It is the last alternative you should be considering, and even then, there’s inadequate evidence that it could produce a significant, lasting change and pain relief.
A 2012 review of 27 clinical studies where the runner’s knee was treated with surgical intervention reported “no additional improvement in PFP symptoms and function over 9 months after surgery.”
And even for hand-picked patients who were considered good candidates for the surgery, failure rates of 20-30% have been reported.
Shin splints or “medial tibial stress syndrome”
The shinbone (medical term—tibia) is the major bone connecting your knees to the feet. When an inflammation occurs in the muscles, tendons, and bone tissue around your tibia, patients feel sharp to aching pain—a condition called shin splints. Shin splints can often be an early sign of a developing stress fracture or a condition called exertional compartment syndrome.
Much like runner’s knee, shin splints develop due to repetitive stress and overuse of the shinbone. Any activity that involves repetitive leg movements (jogging, swimming, cycling, tennis, hiking) can contribute to the condition.
Shin splints often occur after an aggressive change in the patient’s exercise patterns. For example, when patients dive head-first into a new sport or dramatically increase the load of their current exercises—that’s when the pain in the calves usually appears.
The pain is “sharp and razor-like or dull and throbbing.” It may surface during or after the exercise and can be aggravated by touching the sore spot.
Surgery is only employed to treat shin splints in cases where the patient does not respond to non-surgical treatment. The effectiveness of surgery for shin splints is unclear. The surgery involves opening the fascial plane to allow for more space.
How to Prevent Injury for Joggers?

While there’s no hard evidence as to whether all running-related injuries can be prevented, there are several proactive steps that can benefit a jogger:
- Regularly buy shock-absorbing footwear: For jogging, you want to equip yourself with shoes that are highly shock-absorbant. According to the American Academy of Orthopaedic Surgeons, running shoes lose 60% of their shock-absorbing qualities after 250 to 500 miles of running, so people who run 10 miles per week should consider replacing their footwear after 9-12 months of use. When choosing your running shoes, you also want to opt for ones that provide stability and cushion for your foot.
- Choose the right running surface: The environment you jog in is important and not just the weather conditions — the surface your feet are repetitively hitting is just as important. Soft surfaces, like a running track, grass or dirt are least shock-inducing, thus least detrimental for your joints. Avoid running in the hills, as the upwards/downwards angle is damaging to your body. If you’re running on a track or other curving trajectory, make sure to switch the direction you’re running to make sure you have pressure on both feet.
- Try barefoot running: Barefoot running has been gaining popularity among regular joggers. Barefoot running is unlikely to solve knee problems, but many people claim that the practice has helped them fix shin splints and reduce foot pain. The idea behind it is that barefoot running helps spread out the pressure across the entire lower leg and trains a wider range of supportive leg muscles.
- Make incremental changes: While a “just-do-it” attitude may do wonders for your motivation, our bodies don’t appreciate sudden changes. In terms of increasing your exercise intensity or the range of exercises performed, always strive for baby-step changes. This way, you’ll give your body the time it needs to adjust and avoid overuse.
- Rest: Most problems associated with running and other sports that lead to leg overuse are caused by inflammation in certain parts of your legs. The best solution is to simply give your body enough time to rest and heal.
- Do cross-sport exercise: One of the best things you could do to prevent injury is to train your body in cross-discipline sports. If you’re a runner, for example, start actively swimming—at least once a week. If you play tennis, go for low-weight strength exercises. Consult a physician to develop a cross-discipline exercise regimen that will benefit you the most.
Regenerative Treatments for Jogging Injuries
If conventional treatments don’t ease your pain, your healthcare provider may suggest regenerative therapies or orthobiologic methods. These are non-invasive and less painful alternatives for surgical treatments with a shorter recovery time.
The aim is to reconstruct the damaged tissues in the injury site by injecting healthy cells from other parts of the patient’s body. One great benefit of orthobiologic treatments is that they are outpatient procedures, so you can go home right after the process.
Typically, there are two types of regenerative therapies performed at CELLAXYS:
Platelet-Rich Plasma (PRP) Therapy
PRP therapy isolates platelets from the patient’s plasma and makes them concentrated. Then, the platelets are reinjected into the patient’s injury site to promote healing. Platelets are the healing components of our body that encourage healing and form clots after injuries.
Platelets perform three important functions to boost your healing mechanism. First, they release 10 Growth Factors to promote the growth of healthy tissues. Second, they send chemical impulses to attract growth cells from the blood. Third, they produce fibrin, a sticky web-like structure that serves as the scaffolding for the growth of new and healthy tissues.
The presence of a high number of platelets in the injury site indicates faster recovery and healing. PRP has been popular in treating the spine, sports, and orthopedic injuries. The procedure only takes around 45 minutes to complete.
Cell-Based Therapies
These are also known as stem-cell therapies. This orthobiologic treatment focuses on replacing the patient’s damaged cells or tissues with their healthy cells, called “autologous tissues.” The doctor examines the injury site, extracts healthy cells from any part of your body, and reinjects them into the damaged area.
There are two types of cell-based therapies for different injuries.
- Minimally Manipulated Adipose Tissue transplant (MMAT). The procedure takes healthy cells from your adipose (fat) tissues, processes them, and then reinjects them into the injured areas. If you have injuries in multiple places when running, the doctor can perform MMAT in all these locations in the same process.
- Bone Marrow Concentrate (BMAC). This method harvests highly concentrated cells from your healthy bone marrow and injects them into the injury site.
The doctor puts the patients under anesthesia during both of these cell-based therapies. They will use a live X-ray and ultrasound to identify the right spots of jogging injuries. MMAT and BMAC both take around 1.5-2 hours to complete. Patients report quick healing from these treatments.
Sources
Footnotes
- Collins NJ, Bisset LM, Crossley KM, Vicenzino B. Efficacy of nonsurgical interventions for anterior knee pain: systematic review and meta-analysis of randomized trials. Sports medicine. 2012;42:31-49.
- Hiemstra LA, Kerslake S, Irving C. Anterior knee pain in the athlete. Clinics in sports medicine. 2014;33(3):437-59.
- Aguib Y, Al Suwaidi J. The Copenhagen city heart study (Østerbroundersøgelsen). Global Cardiology Science and Practice. 2015;2015(3):33.
- Nielsen RO, Buist I, Sørensen H, Lind M, Rasmussen S. Training errors and running related injuries: a systematic review. International journal of sports physical therapy. 2012;7(1):58.
- Kannus P, Aho H, Järvinen M, Nttymäki S. Computerized recording of visits to an outpatient sports clinic. The American Journal of Sports Medicine. 1987;15(1):79-85.
- LaBella C. Patellofemoral pain syndrome: evaluation and treatment. Primary Care: Clinics in office practice. 2004;31(4):977-1003.
- Halabchi F, Abolhasani M, Mirshahi M, Alizadeh Z. Patellofemoral pain in athletes: clinical perspectives. Open access journal of sports medicine. 2017:189-203.
References
- Shin Splints. OrthoInfo. Accessed 2/25/2024.
- Tips for a Safe Running Program. OrthoInfo. Accessed 2/25/2024.
- Taking the pain out of runner’s knee. Harvard Health Publishing. Accessed 2/25/2024.
CELLAXYS does not offer Stem Cell Therapy as a cure for any medical condition. No statements or treatments presented by Cellaxys have been evaluated or approved by the Food and Drug Administration (FDA). This site contains no medical advice. All statements and opinions are provided for educational and informational purposes only.
Dr Pejman Bady
Author
Dr. Pejman Bady began his career over 20 years ago in Family/Emergency Medicine, working in fast-paced emergency departments in Nevada and Kansas. He has served the people of Las Vegas as a physician for over two decades. Throughout this time, he has been met with much acclaim and is now the head of Emergency Medical Services in Nye County, Nevada. More about the doctor on this page.
Dr Pouya Mohajer
Contributor
Pouya Mohajer, M.D. is the Director of Spine and Interventional Medicine for CELLAXYS: Age, Regenerative, and Interventional Medicine Centers. He has over 20 years of experience in pain management, perioperative medicine, and anesthesiology. Dr. Mohajer founded and is the Medical Director of Southern Nevada Pain Specialists and PRIMMED Clinics. He has dedicated his career to surgical innovation and scientific advancement. More about the doctor on this page.