Published on: November 28, 2018 | Updated on: November 5, 2024
Runner’s knee is a general term for several conditions that cause knee pain and is a common issue among highly-active adults.
Constant physical strain and poor running form induce and exasperate the conditions necessary for the problem to start, and once it’s begun, it can be difficult to combat. Though runner’s knee is most prevalent among highly-active individuals, it is still a concern for less active people who have suffered some form of knee trauma in the past.
Additionally, runner’s knee can escalate into more severe issues if left unchecked. While there are treatments, most of these solutions only help to reduce the speed at which these knee issues escalate. Thankfully, breakthroughs in regenerative health services – such as those offered at Cellaxys – are paving the way for more permanent solutions.
What Is Runner’s Knee?

While runner’s knee is a general term for knee issues related to knee fatigue induced by physical aggravation, there are 3 conditions most associated with the term – iliotibial band syndrome (ITBS), patellofemoral pain syndrome (PFPS), and patella tendonitis.
Iliotibial Band Syndrome (ITBS)
Characterized by pain on the sides of the knee, this is the term used to describe a fatigued or worn-out iliotibial band. The iliotibial band is a thick band of connective tissue which extends from the insides of the bottom of the knee, and up to the pelvis and hips.
Repetitive flexion and extension of the knee during running causes the band to rub over the lateral femoral epicondyle (the bone directly behind and above the knee) and may lead the area to become inflamed.
Over time, as protective tissues are worn away, the pain from this inflammation may become more and more severe, to the point of a drastic reduction in mobility.
Patellofemoral Pain Syndrome (PFPS)
Characterized by pain on the front of the knee, around and under the kneecap, PFPS is the most common type of runner’s knee and extends far beyond the scope of runners. Hikers, cyclists, basketball players, and even people who sit for a living (leaving the knee constantly flexed can fatigue the kneecap), may all experience a type of PFPS, albeit at different levels of severity.
Patellar Tendonitis
Characterized by pain under or behind the knee cap, patellar tendonitis affects the patella tendon which attaches the main shin bone (tibia) to the knee cap (patella).
This tendon takes the forces of running, jumping, and walking with every step and carries a huge amount of force every day. This is often referred to as “jumper knee”. The tendon can become inflamed and painful often with coexisting tears or micro-tears.
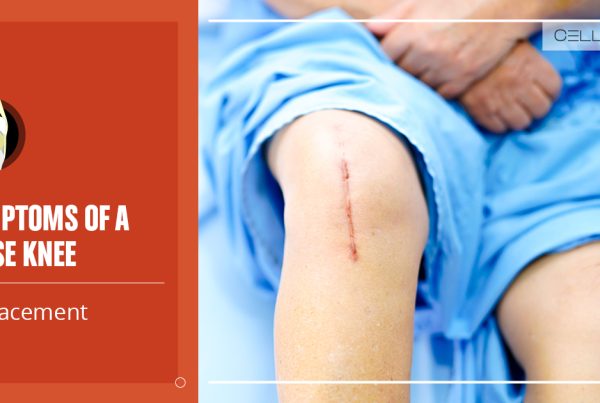
Runner’s Knee: Symptoms
Here are some common symptoms of runner’s knee:
- Dull but aching pain around the kneecap increases when you bend the knee and run, squat, or walk downhill.
- Lasting pain that doesn’t end.
- Pain gets worse after a workout session and lasts for days.
- Discomfort and pain when you sit with the legs hanging down and knees bent.
- Popping or clicking sound whenever you bend your knee.
- Swelling and tenderness around the kneecap.
What Causes Runner’s Knee?
Though the most common contributing factor to runner’s knee is vigorous physical activity, there are many underlying reasons a person may begin to suffer from this condition.
The knee is made up of a complex network of cartilages, fats, ligaments, tendons, muscles, and bones which act together to provide fluid motions when walking. In time, some of these components can be worn down or stressed to the point of fracture or tear.
Doctors haven’t reached a consensus on the range of causes for these erosions or tears, but they agree that repetitive cycles of tightening and relaxing this area along with some forms of inflammation can aggravate these tissues and cause some of the symptoms of runner’s knee.
Additionally, trauma to the knee, flat feet, arthritis, and weak thigh muscles have also been linked to problematic knee function.
Whatever the mechanism at work, when the condition begins, nerves start to sense pain in the soft tissues and bones that surround the kneecap. Over time, the severity of this pain increases, and the conditions to induce it become milder.
If walking up or down slopes, squatting, or simply resting with the knee bent causes knee pain, then it may be time to examine your knee health or seek out professional advice.
What Type of Runner’s Knee Do I Have?
Before treatment can occur, it is best to identify the source of your runner’s knee as treatments vary based on the origin of the pain. While the best possible way to diagnose the issue is to see a trained physician, you may want to do a preliminary check on your own.
Below are some guidelines which may help you distinguish between the 3 most common knee issues:
ITBS
- Pain is derived from the side of the knee. While pain can be experienced anywhere in the general vicinity of the knee, the focal point is always on the sides.
- Pain is not induced when poking the kneecap, but rather the side of the knee, especially right under the knee at either end of the cusp of the cap.
- Pain is worse when moving down a set of stairs or hills and is noticeably less when moving upwards.
- Pain doesn’t slowly escalate throughout the day but initiates sharply at once (although for ITBS, it can do both).
- Deep knee-bends do not cause sharp pain.
- No obvious damage to the structural integrity of your general knee area.
PFPS
- Pain is derived from under or around the kneecap. While pain can be experienced anywhere in the general vicinity of the knee, the focal point is always on the kneecap.
- Discomfort is experienced when pressing on the kneecap.
- Pain is worse when moving up a set of stairs or hills and is noticeably less when moving downwards, though it may be equally painful doing both.
- The pain escalated slowly, over months and years, and gets gradually worse throughout the day.
- Deep knee-bends cause sharp pain.
- Pain is worse when sitting and once standing up, takes time to go down.
- Obvious structural integrity issues such as knock-knees, flat feet, or kneecaps that are at an angle.
Patellar Tendonitis
- Pain can be both sharp or dull at rest.
- Squatting or jumping can be extremely painful.
- Swollen at or below the level of the knee cap.
- Pain is worse with vigorous activity.
- Stairs can be debilitating from the pain in the front of the knee.
Can Runner’s Knee Cause Permanent Damage?
If left unchecked, runner’s knee can lead to more severe issues throughout the rest of a person’s life.
Constant strain on the knee – be it from poor running form, flat feet, a previous trauma, or other factors – can cause erosion in the soft tissues within the knee. Our bodies do not have the mechanisms available to repair and replenish our supply of some of these soft tissues.
As these tissues are worn away, bones can begin to rub together, nerves can be pinched, and muscles can become awkwardly strained. These conditions only worsen over time and the knee pain they cause can become increasingly severe to the point of debilitation.
Without proper treatment and consultation, runner’s knee can cause several permanent issues.
How Do I Stop Runners Knee?
Runner’s knee (and the issues associated with it) becomes incrementally worse if the proper treatments or modifications aren’t made early on. The earlier a person begins to combat the habits which cause runner’s knee, the more fruitful these efforts will be.
To “stop” runner’s knee, the first step is to correctly diagnose your specific issue. Below is a simple outline of the steps you should take:
1. Identify the source of the pain
Is it coming from the front of the knee, sides, or neither? You can use this information to identify the source of your issue and develop a treatment routine specific to the problem. While most knee issues have similar solutions, each condition also has a specific set of treatments that target individual problem areas.
2. Focus on your movements throughout the day
Which activities or parts of your daily routine seem to cause flare-ups? If a specific activity, be it running, jumping, squatting, or resting, seems to especially upset your knees, stop doing it or find a way to do it that causes less strain for the knees. Make sure to avoid these activities for a while. Even after your knee seems to feel better, it may not have fully recovered enough to resume your routine.
3. Develop better habits for preventing flare-ups
With the problem area and pain-inducing movements uncovered, either eliminate the specific movement from your routine or consult a professional for developing a better method of approaching that routine.
If it is part of your workout, a personal trainer may be able to help you identify problems with your form. If the issue stems from a part of your job, you may want to consider buying a knee brace or shoe insoles. Anti-inflammatory medications may be another avenue to pursue, though these treatments often have unwanted side effects and become less effective over time.
How to Prevent Runner’s Knee
You will need a comprehensive workout plan to prevent a runner’s knee from recurring. The plan should include a combination of strength training exercises, listening to your body’s cues, and biomechanics.
Here are some tips to keep safe from runners knees:
Strengthen Your Muscles
Weak muscles are more prone to pain, increasing the risk of Runner’s knee. Work on building your quadriceps, hamstrings, and hip muscle strength. When these muscles are strong, you’ll exert less pressure on the knee joint. Make leg raises, hip bridges, and other exercises part of your daily workout routine.
Stretch these muscles, keep them flexible, and avoid sudden jumps in your training or workout schedule.
Focus on Running Form
Your posture is crucial in preventing Runner’s knee and other pains. Keep a proper form when running or working out. Do not slouch or exert more pressure than necessary on your feet to avoid injuring the knee. Run on the midfoot rather than the heel or toes.
Keep the stride short, too.
Footwear
Even though many people don’t give much thought to it, footwear is key to keeping your feet from getting injured or exerting too much pressure on any body parts. Wear proper running shoes that support the arch.
If you have flat feet, get customized orthotics for better support.
How Do I Recover From Runner’s Knee?
Many people wonder if it is possible to heal completely from runner’s knee. With the constant strain from movement, runner’s knee can be an especially difficult affliction to recover from.
So, how do you heal from runner’s knee? There are several options for runner’s knee treatment and rehabilitation, some of the most common include:
1. Stretches
Knee pain can originate from tightness in the muscles and tendons connected to the knee. Hips, hamstrings, glutes, quads, and calves all work together to provide movement in the knee and when one is jeopardized, the others are affected. To reduce the strain and pain in the knee, you must reduce the tension in all of these areas.
Practice various stretches on the different muscle groups and tendons mentioned above. Make sure to hold them for 30-60 seconds for maximum effect. You may also consider buying a foam roller or elastic band to help provide deeper stretches. While stretching won’t eliminate the problem, it will provide immediate relief from the occasional flare-up.
2. Massage
Either self or professional, massage is a great way to improve joint mobility and treat pain and stiffness in the knee. A controlled trial analyzed the effectiveness of self-massage in treating pain and stiffness and increasing physical function in 40 adults diagnosed with knee osteoarthritis.
The study found that participants who gave themselves a 20-minute massage twice a week showed significant improvement in their pain.
Performing deep, gliding massage strokes helps to soften and lengthen muscle fibers within the knee. Additionally, using knuckles, forearms, and elbows to target specific problem areas can help make this form of treatment more effective.
You may also tap the knee area to stimulate circulation and warm soft tissue. Another technique involves pressing the fingers firmly into the soft tissue around the knee and moving the tissue back and forth using short strokes.
3. Strength training
Well-trained supporting muscles can help cushion the force being applied to the knee and thus reduce knee pain that is associated with high-impact activities. While strengthening these groups won’t eliminate the pain outright, it will benefit your knee’s health in the long run. Weak supporting muscles place strain in the knee area and thus wear away at the cushioning cartilages of the knee.
As these cartilages wear away, your nerves will become more and more exposed, and thus, your pain will become sharper and sharper. With a strong supporting system of muscles, the knee takes less of the strain and the cartilage remains intact for longer.
Focus on working groups such as the glutes (butt muscles), the lumbar spine, and quadriceps (specifically the vastus medialis, or, “VMO”) in order to help support the efforts of your knees.
4. Corticosteroid injections
Cortisone helps to suppress the immune system, reducing inflammation and pain at the site of an injury. Corticosteroid injections work very quickly as opposed to the other treatments mentioned above. The benefits derived from these injections are short-term though and typically last anywhere from 6 to 12 weeks.
Doctors agree that while these injections are valuable for the occasional flare-up, long-term use of corticosteroids presents many risks and often gives less relief the longer they are used. Cortisone degrades tissues and can ultimately lead to worse pain and irreparable damage. Professional athletes began moving away from these injections with the advent of PRP and cell-based therapies. The general public has now done the same.
5. Ice and Elevation
Apply ice to the knee every few hours for 15-20 minutes. This will prevent swelling and pain. Keep your knee raised to reduce inflammation and pain.
6. Platelet-rich plasma (PRP) therapy
Platelet-rich plasma (PRP) therapy has been used as regenerative medicine for decades. In this process, the healthcare provider isolates the platelets from the patient’s blood plasma, concentrates them, and then re-injects them into the injured knees.
Platelets are responsible for promoting healing in our bodies. They release 10 Growth Factors to accelerate the development of healthy tissues and cells. They also send chemical signals to attract growth cells in the blood and create a web-like scaffolding called fibrin. Fibrin supports the growth of healthy cells and shortens the recovery period.
PRP is an outpatient procedure, so you may go home right after the procedure, which takes about 45 minutes to complete.
7. Cell-based therapies
Also known as stem cell therapy, cell-based therapies help regenerate cartilage tissue in the knee, which improves knee function and reduces pain. They are performed on your autologous tissues, the cells or tissues that are your own.
Depending on your knee condition, your doctor may go for any of the two types of cell-based therapies:
- Minimally Manipulated Adipose Tissue (MMAT) Transplant. This procedure involves removing healthy cells from your adipose (fat) tissues and re-injecting them into the injured areas of your knees. If the doctor suspects injuries in multiple locations of your knee, they will perform MMAT in all these places in the same procedure.
- Bone Marrow Concentrate (BMAC). This method extracts healthy, highly concentrated cells from your bone marrow and re-inserts them into your knees.
Both of these cell-based therapies are performed under anesthesia. They take around 1.5 to 2 hours to complete, after which you can go home. The doctor will identify the correct location of injury in your knee through live X-rays (fluoroscopy) or ultrasound.
These treatments will eliminate the problem outright and help speed up the recovery process. Both cell-based therapies and PRP begin the healing process by transplanting the necessary ingredients to begin the healing process.
Patients should finish the healing process through exercise and activity. Afflicted people should always consult a doctor or physical therapist for the best treatments for their specific condition.
Sources
Footnotes
- Arroll B, Edwards A. Runner’s knee: what is it and what helps?. The British Journal of General Practice. 1999;49(439):92.
- Atkins DV, Eichler DA. The effects of self-massage on osteoarthritis of the knee: a randomized, controlled trial. International journal of therapeutic massage & bodywork. 2013;6(1):4.
- Pretorius DM, Noakes TD, Irving G, Allerton K. Runner’s knee: What is it and how effective is conservative management?. The Physician and Sportsmedicine. 1986;14(12):71-81.
- Mellinger S, Neurohr GA. Evidence based treatment options for common knee injuries in runners. Annals of translational medicine. 2019;7(Suppl 7).
- Pountos I, Panteli M, Walters G, Bush D, Giannoudis PV. Safety of epidural corticosteroid injections. Drugs in R&D. 2016;16:19-34.
References
- Knee Anatomy. ARTHRITIS-Health. Accessed 2/25/2024.
- Patellofemoral Pain Syndrome (Runner’s Knee). Johns Hopkins Medicine. Accessed 2/25/2024.
- Runner’s Knee: What You Need to Know. WebMD. Accessed 2/25/2024.
- Runner’s Knee. Healthline. Accessed 2/25/2024.
CELLAXYS does not offer Stem Cell Therapy as a cure for any medical condition. No statements or treatments presented by Cellaxys have been evaluated or approved by the Food and Drug Administration (FDA). This site contains no medical advice. All statements and opinions are provided for educational and informational purposes only.
Dr Pouya Mohajer
Author
Pouya Mohajer, M.D. is the Director of Spine and Interventional Medicine for CELLAXYS: Age, Regenerative, and Interventional Medicine Centers. He has over 20 years of experience in pain management, perioperative medicine, and anesthesiology. Dr. Mohajer founded and is the Medical Director of Southern Nevada Pain Specialists and PRIMMED Clinics. He has dedicated his career to surgical innovation and scientific advancement. More about the doctor on this page.
Dr Pejman Bady
Contributor
Dr. Pejman Bady began his career over 20 years ago in Family/Emergency Medicine, working in fast-paced emergency departments in Nevada and Kansas. He has served the people of Las Vegas as a physician for over two decades. Throughout this time, he has been met with much acclaim and is now the head of Emergency Medical Services in Nye County, Nevada. More about the doctor on this page.