Published on: January 24, 2020 | Updated on: August 29, 2024
The rotator cuff is a group of muscles and tendons in the shoulder that allow us to freely move our shoulders. Sustaining any damage to this area of the body can be cause for alarm, as these injuries typically lead to debilitating symptoms.
Pain, stiffness, and complete loss of function are some of the most common signs of a rotator cuff injury.
Many patients turn to surgical intervention if their injuries are acute enough. Unfortunately, many of the people opting for surgery have no idea what to expect which can greatly reduce the success rate of their treatment.
Rotator Cuff Anatomy
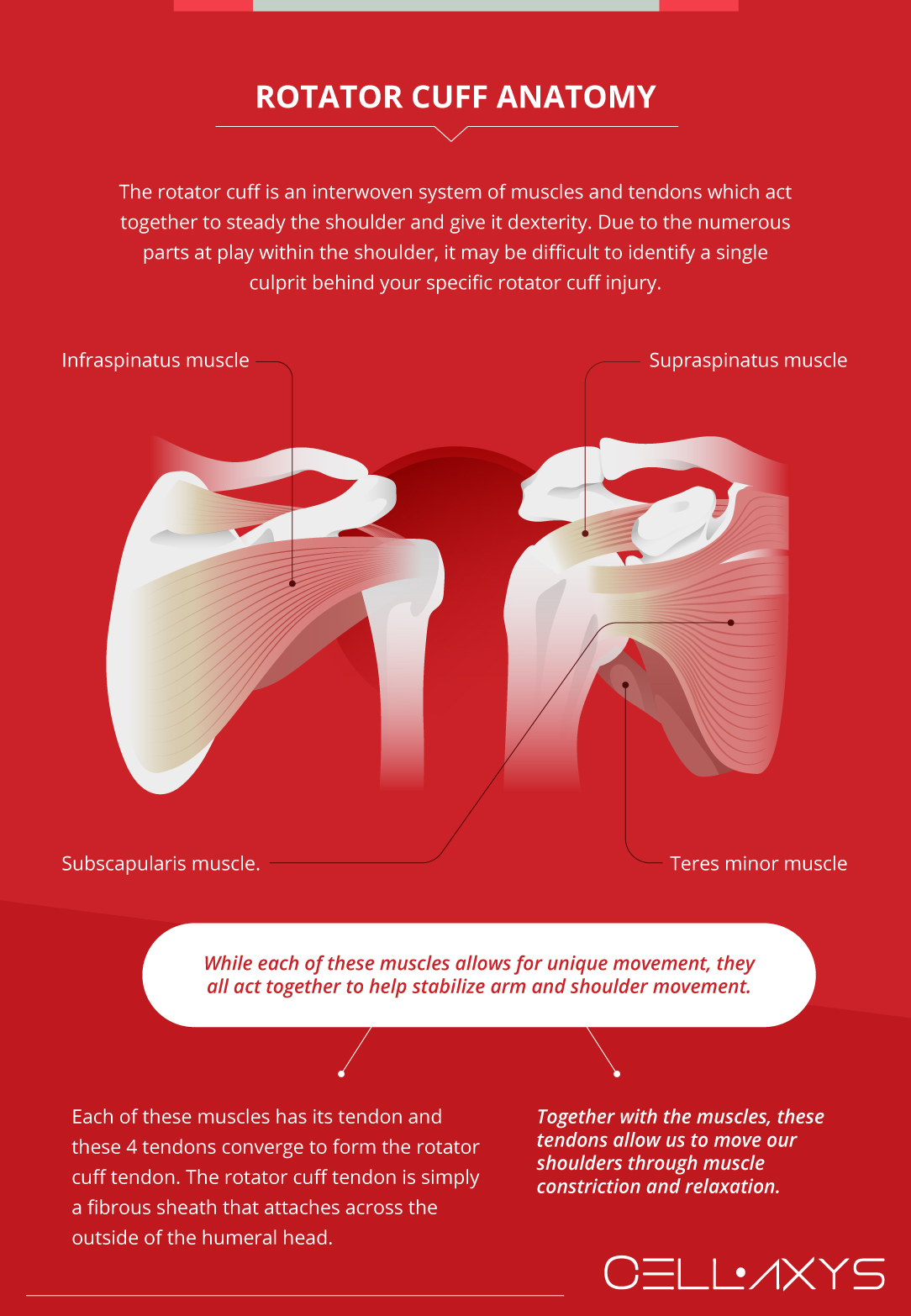
The rotator cuff is an interwoven system of muscles and tendons which act together to steady the shoulder and give it dexterity. Due to the numerous parts at play within the shoulder, it may be difficult to identify a single culprit behind your specific rotator cuff injury.
The shoulder is a ball and socket joint, wherein a “ball”, in this case, the head of the humerus (arm bone), rests in the “socket” of the shoulder (a bone known as the scapula).
This design allows for a high dexterity to stability ratio when combined with the numerous muscles which surround the bones and the tendons which tether the bones to the muscle.
7 muscles surround the shoulder, in anatomical terms, these are known as the scapulohumeral muscles. Of these 7, only 4 make up the rotator cuff – the supraspinatus muscle, the infraspinatus muscle, teres minor muscle, and the subscapularis muscle. While each of these muscles allows for unique movement, they all act together to help stabilize arm and shoulder movement.
Each of these muscles has its tendon and these 4 tendons converge to form the rotator cuff tendon. The rotator cuff tendon is simply a fibrous sheath that attaches across the outside of the humeral head. Together with the muscles, these tendons allow us to move our shoulders through muscle constriction and relaxation.
One of the more common rotator cuff injuries is a tear. These tears can occur following acute trauma or may be due to degenerative effects over time. Patients will feel a drastic reduction in the range of motion, pain, swelling, and instability following a rotator cuff tear.
Rotator cuff injuries are most common in people over the age of 60 or who express repeated overhead motions. Athletes, drummers, and workers whose jobs entail long bouts of physical exertion involving the shoulder are most susceptible to these types of injuries.
Diagnosing Rotator Cuff Tears
After an acute injury or at the onset of the above-mentioned symptoms, you should have a trained health team perform a diagnosis of your rotator cuff. These assessments can help a person prevent further damage and ensure that proper treatment takes place.
Initial Check-Up
Doctors will run a routine medical background check to uncover any past trauma which may be causing symptoms. They will follow this up with a physical examination.
Physical examinations for rotator cuff tears are simple – doctors will stretch the arm and shoulder to the outer limits of their range of motion and palpate the area to uncover any peculiarities. These tests will help doctors pinpoint an exact location for the tear to help assure the medical imaging tests cover the correct portion of the shoulder.
Medical Imaging
If the initial tests confirm an issue, doctors will move on to a range of imaging tests. These tests will provide an inside view of the structures within the shoulder and give doctors more insight into what may be causing the problem. Standard imaging tests include:
- MRI: Using radio waves and magnetic fields, doctors can take detailed pictures of your shoulder.
- X-rays: Will show doctors whether the humeral head is pushing into the rotator cuff space and creating the symptoms of a rotator cuff tear.
- Ultrasound: Allows doctors to check the soft tissues (muscles and tendons) in your shoulder.
If a rotator cuff tear is found, and the injury is acute enough, doctors will recommend surgical intervention. While rotator cuff surgery is fairly common and comes with minimal risk, many people are still unprepared for what to expect.
To ensure the most success post-surgery, it is best to get an idea of the steps included before, during, and after the procedure.
Rotator Cuff Tear Surgery Recovery Timeline
Surgical intervention for rotator cuff tears is minimally invasive. The shoulder is far enough away from vital organs that risk factors are low and recovery is fairly short. Though a patient may be able to return to work and daily activity immediately (1 to 2 weeks) following surgery, they will not have full function of their shoulder.
Below is some general guidance to prepare you for your rotator cuff surgery:
- Preparing for rotator cuff tear surgery: Successful surgeries begin with adequate preparation. These preliminary steps help ensure patient safety and may be critical in determining the outcome.
- Make sure you understand the type of surgery you are going in for. Each variety of surgery will require different preparatory steps, procedures, and recovery periods.
- Make sure you understand how long the surgery will last – The more tendons affected by an injury, the longer a procedure will take.
- Schedule bloodwork to reduce outside risks such as aversion to anesthetics or unknown blood or autoimmune disorders.
- Arrange for a ride to and from the hospital. Patients undergoing rotator cuff tear surgery will be prescribed medications that may prevent them from driving.
- Prepare a small parcel of luggage for the duration of your hospital stay. Toiletries, entertainment, and clothes may be necessary for the hospital stay.
- Follow your doctor’s orders. If they give a timeline to refrain from eating or drinking, it is important to follow these guidelines as anesthetics may interfere with the body’s natural digestive processes leading to complications during surgery.
- Maintain an adequate sleep schedule to boost the body’s resilience to post-surgical pain and amplify its healing processes.
- Once all preparatory steps are complete, make sure to check into the hospital promptly to ensure doctors have enough time to go through their pre-surgical procedures.
- The procedure: Rotator Cuff tear surgery is typically performed through the aid of minimally invasive tools. Surgery may take a couple of hours, after which doctors will monitor the patient’s vital signs to ensure the body responded well to surgery.
- Patients are typically placed under anesthetic until they fall asleep before surgery.
- If damage is minimal, doctors will begin the surgery with small incisions in the shoulder followed by the insertion of a tiny device known as an arthroscope. The arthroscope creates a small tunnel that burrows through the knee, pushing away surrounding tissues.
- The doctors can place several small tools within the arthroscope to both see what they’re working on as well operate on the tissues directly.
- If the injury is more complex, doctors may opt for an open rotator cuff surgery. This will involve larger incisions and may require various muscles to be moved around to access the damaged area. Recovery from open rotator cuff surgery is typically longer than arthroscopic surgery due to the complexity involved.
- The doctor will either sew the ruptured rotator cuff tendons back together, remove degenerated portions of them and sew them back together, or remove them and replace them completely. The worse the condition of the rotator cuff tendons, the longer the surgery will take.
- Once the surgery is finished, doctors will remove the arthroscope if one was inserted and close the incisions.
- First few hours after surgery: Anesthetic will be applied routinely throughout the first few hours after the surgery. Doctors will monitor vital signs to ensure the surgery was successful. Typically, rotator cuff tear surgery is very low-risk and complications are rare.
- 1-2 days after surgery: Recovery for rotator cuff tear surgery is short. While regular functionality isn’t immediate, patients will be tasked to move within 1-2 days after surgery.
- A physical therapist will be assigned to you and you will begin a routine of light exercise to help stabilize the shoulder.
- Some light weight-bearing activities may be asked of you during these exercises.
- You will be released from hospital care and told to monitor your recovery at home. High fever, excessive bleeding, and escalating pain should be reported to your health care team immediately.
- 1 week after surgery: Patient activity levels will gradually be increased.
- Once the patient is home, they will be asked to follow the routines their physical therapist taught them.
- Creams, ointments, and medication should be taken as routinely as the doctors have prescribed and activity levels should be moderate.
- Simple physical therapy such as light massage and hot/cold treatments can be applied if medication and rest do not help alleviate post-surgical pain. Consult a doctor if the pain becomes excruciating or if you suffer a shoulder injury immediately following surgery.
- After 10 days, the stitches placed to close the wound will be removed and a light-follow up exam will take place.
- 1 month after surgery: Light activities can resume, and physical therapy may intensify.
- At this point, the surgical wounds should be healed and normal activity levels should resume, albeit with minimal pain and discomfort.
- Extended use may cause flare-ups of pain, but these bouts of pain should wane over time as the wounds fully recover.
- 1 year after surgery: By this time the surgical pains should be gone, and normal activity levels should return. While pain and discomfort may be inevitable, these pains should not be so excruciating that they prevent functionality.
- Patients should expect a reduced range of motion as well as reduced stability on the shoulder that was operated on.
- At times, environmental stresses – high elevation, humidity, excess cold/heat – will trigger pain, this is normal and should only be checked on if the pain does not subside once environmental factors have been eliminated.
Before applying surgical intervention to any issue, it may be best to consult specialized medical professionals. There may be alternatives to surgery that a patient should consider.
One treatment that may help repair light rotator cuff tendon damage or reduce recovery periods post-surgery is regenerative therapy.
Rotator Cuff Tears and Regenerative Medicine
Rotator cuff surgeries are subjectively successful. Some studies have shown insufficient evidence to conclude that surgery is more successful at treating rotator cuff tear symptoms than conservative treatments.
Surgical intervention requires medication and physical therapy routines and low activity levels immediately following the procedure. With these side effects in mind, many people turn to regenerative therapies to boost the body’s natural healing processes after sustaining a shoulder injury.
At CELLAXYS, we offer two types of regenerative therapies:
Cell-Based Therapies
Cell-based or stem cell therapies extract cells from the patient’s own tissues or “autologous” tissues, process them, and reinject them into the injury site. Doctors typically take cells from two parts of the patient’s body: adipose (fat) tissue and bone marrow. Depending on your condition, the doctor will opt for one of the two types of cell-based therapies:
- Minimally Manipulated Adipose Tissue (MMAT) transplant: it replaces damaged cells with healthy ones from the patient’s adipose (fat) cells and reinjects them into the injury site after processing. MMAT can be performed in multiple locations in the same procedure.
- Bone Marrow Concentrate (BMAC): it takes highly concentrated cells from the patient’s bone marrow and reinjects them into the injury site.
Both cell-based procedures take about 1.5 to 2 hours to complete.
Platelet-Rich Plasma (PRP) Therapy
PRP therapy uses the body’s natural healing cells called platelets to boost recovery from the injury. The process isolates platelets from the patient’s blood plasma, processes them, and returns them to the injury site.
Platelets contain 10 Growth Factors and release chemical impulses to draw fresh tissues to the site of an injury. They also produce web-like support for the development of new tissues called fibrin. PRP is a popular orthopedic procedure for treating many injuries. The process is completed in 45 minutes.
Cell-based and PRP therapies are performed as an outpatient procedure, so you can go home after the treatment. The doctor uses live X-rays and ultrasounds to detect the exact transplant location.
By using these therapies in unison, many patients have found relief from post-surgical symptoms and found that their recovery processes take much less time.
If you want to learn more about how regenerative therapies can help you, contact the CELLAXYS offices today to set up a consultation.
Sources
Footnotes
- Wu JG, Bordoni B. Anatomy, Shoulder and Upper Limb, Scapulohumeral Muscles. StatPearls Publishing, Treasure Island (FL). 2019.
- Fermont AJ, Wolterbeek N, Wessel RN, Baeyens JP, De Bie RA. Prognostic factors for successful recovery after arthroscopic rotator cuff repair: a systematic literature review. Journal of Orthopaedic & Sports Physical Therapy. 2014;44(3):153-63.
- Kurowicki J, Berglund DD, Momoh E, Disla S, Horn B, Giveans MR, Levy JC. Speed of recovery after arthroscopic rotator cuff repair. Journal of shoulder and elbow surgery. 2017;26(7):1271-7.
- Manaka T, Ito Y, Matsumoto I, Takaoka K, Nakamura H. Functional recovery period after arthroscopic rotator cuff repair: is it predictable before surgery?. Clinical Orthopaedics and Related Research. 2011;469:1660-6.
- Conti M, Garofalo R, Delle Rose G, Massazza G, Vinci E, Randelli M, Castagna A. Post-operative rehabilitation after surgical repair of the rotator cuff. Musculoskeletal Surgery. 2009;93:55-63.
References
- Rotator cuff injury. Mayo Clinic. Accessed 2/25/2024.
- Failed Rotator Cuff Repairs. Johns Hopkins Medicine. Accessed 2/25/2024.
- Rotator Cuff Surgery: Arthroscopic Repair of a Torn Rotator Cuff. HSS. Accessed 2/25/2024.
- Rotator Cuff Surgery: A Timeline for Recovery. Healthline. Accessed 2/25/2024.
CELLAXYS does not offer Stem Cell Therapy as a cure for any medical condition. No statements or treatments presented by Cellaxys have been evaluated or approved by the Food and Drug Administration (FDA). This site contains no medical advice. All statements and opinions are provided for educational and informational purposes only.
Dr Pejman Bady
Author
Dr. Pejman Bady began his career over 20 years ago in Family/Emergency Medicine, working in fast-paced emergency departments in Nevada and Kansas. He has served the people of Las Vegas as a physician for over two decades. Throughout this time, he has been met with much acclaim and is now the head of Emergency Medical Services in Nye County, Nevada. More about the doctor on this page.
Dr Pouya Mohajer
Contributor
Pouya Mohajer, M.D. is the Director of Spine and Interventional Medicine for CELLAXYS: Age, Regenerative, and Interventional Medicine Centers. He has over 20 years of experience in pain management, perioperative medicine, and anesthesiology. Dr. Mohajer founded and is the Medical Director of Southern Nevada Pain Specialists and PRIMMED Clinics. He has dedicated his career to surgical innovation and scientific advancement. More about the doctor on this page.