Published on: August 22, 2019 | Updated on: August 29, 2024
Table of contents
- Intro
- Anatomy of the Flexor Hallucis Longus
- Flexor Hallucis Longus Pain Causes
- Signs and Symptoms of Flexor Hallucis Longus Pain
- Diagnosis of Flexor Hallucis Longus Pain
- Conventional Treatments for Flexor Hallucis Longus Pain
- Activity Modification and Load Management
- Regenerative Medicine and Flexor Hallucis Longus Pain
The flexor hallucis longus is one of a group of deep muscles in the lower leg and foot. This particular muscle is prone to injury and degeneration due to its location, application, and daily use.
Flexor hallucis longus pain is known to reduce mobility and may at times become paralyzing due to the severity of discomfort experienced by those who suffer from it.
Do you have Flexor Hallucis Longus Pain?
Fill out the form below to schedule your FREE virtual consultation
Anatomy of the Flexor Hallucis Longus
The flexor hallucis longus is a muscle that is nested in the back of the leg and is covered by several other muscle groups. The group surrounding this group of deep muscle is known as the “superficial muscle group” and helps to insulate the softer muscles nested inside.
The flexor hallucis longus is responsible for flexing the joints of the big toe. To help accomplish these bends and allow you to perform other functions, the flexor hallucis longus needs a nerve supply. Nerves direct signals from the brain to help stimulate muscle movement.
For the flexor hallucis longus, this supply of synapses comes from the tibial nerve – a nerve that weaves from the upper back portion of the knee, all the way down to the base of the foot and the big toe.
For the flexor hallucis longus, the beginning is along the fibula, a long, thin, and lateral bone in the lower leg. It keeps running along the fibula and connects to the bottom portion of the other lower leg bone, the tibia. Finally, it travels through small grooves in the bones at the back of the foot and ankle and ends as a tendon at the base of the big toe.
By weaving around the ankle and base of the foot, the flexor hallucis longus and its tendon function as a sort of pulley system which contracts and relaxes to provide movement to the big toe and the force to push off from the base of the foot. This intricate weave of tendon and muscle is a common source of pain due to the abnormal compression and stress which is placed on it in daily movement.
Flexor Hallucis Longus Pain Causes
By interacting with its tendon counterpart and the joints of the foot, the flexor hallucis longus can provide movement by pushing the force of the rear foot to the big toe. Over time, the muscle and tendon of the flexor hallucis longus can begin to develop pain due to several reasons. Some of the most common contributing factors for flexor hallucis longus pain are:
- Past injury
- Repetitive exertion
- Hyperextension
- Muscle tears
- Bone constriction
- Weak blood flow
- Abnormal healing after injury
Because of the mechanics which lead to the onset of flexor hallucis longus pain, it is most prevalent in athletes. These types of injuries have come to be known as “dancers tendonitis” due to their extreme prevalence in classic ballet dancers. Swimmers, footballers, gymnasts, sprinters, and anyone who repetitively pushes off from the base of their big toe can also suffer from dancer’s tendonitis and general flexor hallucis longus pain.
Signs and Symptoms of Flexor Hallucis Longus Pain
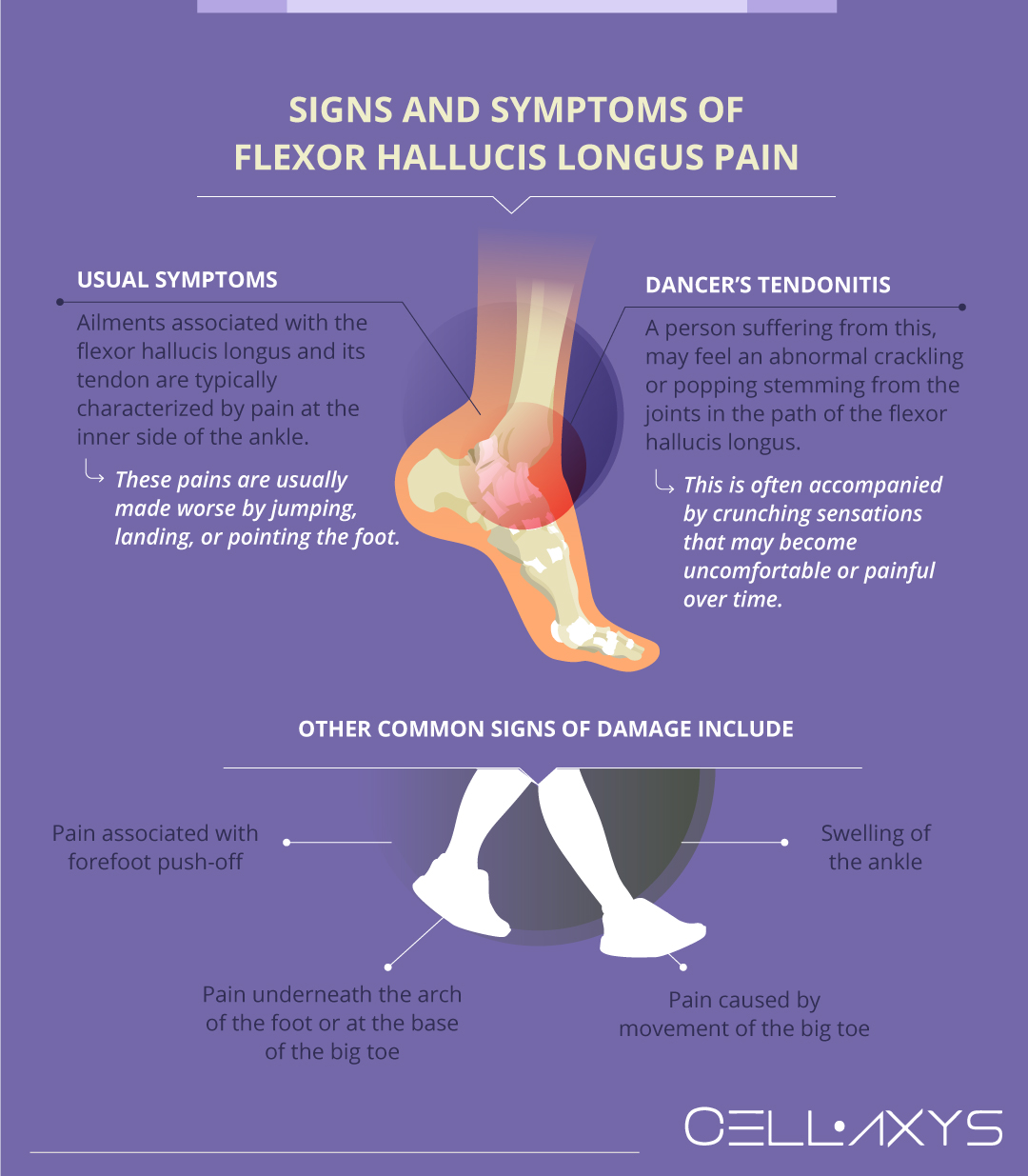
Ailments associated with the flexor hallucis longus and its tendon are typically characterized by pain at the inner side of the ankle. These pains are usually made worse by jumping, landing, or pointing the foot.
A person suffering from dancer’s tendonitis may feel an abnormal crackling or popping stemming from the joints in the path of the flexor hallucis longus. This crackling and popping may be faint or loud enough for others to hear and is often accompanied by crunching sensations that may become uncomfortable or painful over time.
If the symptoms escalate, they may lead to an inability to relax the big toe resulting in a feeling of the big toe being stuck in flexion.
Other common signs of flexor hallucis longus damage include:
- Pain associated with forefoot push-off
- Pain underneath the arch of the foot or at the base of the big toe
- Swelling of the ankle
- Pain caused by movement of the big toe
These signs and symptoms are only a base for the diagnosis of flexor hallucis longus pain, the only way to be certain that there is any damage is to set up a professional medical screening.
Diagnosis of Flexor Hallucis Longus Pain
A clinical examination of a suspected flexor hallucis longus injury includes an inspection of the areas surrounding this muscle and tendon. The regions which yield the most insight into the injury include the back and inner side of the ankle, the underside of the foot, and the sesamoids (bones before the base of the big toe).
First, an examiner will ask the patient to extend the foot to ensure that the flexor hallucis longus is under tension. Next, the examiner will begin to feel for abnormalities in the aforementioned regions, an act known as palpation. By massaging these portions of the foot while the flexor hallucis longus is under strain, an examiner can get an idea of the epicenter of the pain.
Typically, an examiner will look for tenderness in specific locations of the foot or while the foot is under specific positions. These positions are meant to cause increased pressure in the pathways of the flexor hallucis longus and illicit the type of pain response associated with dancer’s tendinitis. This tenderness coupled with a reduced range of motion may be all an examiner needs to accurately deduce flexor hallucis longus injury.
If flexor hallucis injury is suspected, an ultrasound and MRI can provide further insight and a more accurate assessment of the damage around the flexor hallucis longus.
Conventional Treatments for Flexor Hallucis Longus Pain
Pain in the flexor hallucis longus and the associated tendon can be managed or treated in several ways. While most of the following treatments cannot completely eradicate the pain, they can help achieve some measure of comfort for those suffering from it.
Exercise
Perhaps the most common of the treatments on this list, exercise helps to alleviate pressure around the flexor hallucis longus and strengthen the supporting muscles around it. Oftentimes, the exercises are part of a progressing training regimen designed to guide the patient through many levels based on their stage in the recovery process.
This progression is usually based on the amount of load that the flexor hallucis longus can tolerate without inducing the pain being treated.
Most of the exercises used in flexor hallucis longus treatment involve periodically flexing and relaxing the injured muscle. Typical exercises include:
- Resisted plantar flexion of the big toe: an elastic band is looped around the big toe and gets tugged towards the patient to induce a flexed state in the flexor hallucis longus.
- Marble pickups: a patient uses their fourth and big toes to pick a small object off the floor and drop it into a nearby receptacle.
- Towel scrunches: a towel is laid flat on the floor and the patient uses their big and fourth toes to “scrunch” it up while lifting their heel off the floor.
- Tiptoe: a patient will plant a single foot on the floor and raise the other leg while shifting their weight between the base of the big toe and the heel. The patient may be asked to flex their big toe in addition to this exercise.
Activity Modification and Load Management
Along with exercise, activity modification can be of great importance to those suffering from flexor hallucis longus pain. By guiding patients into new habits, physical therapists can help patients reduce the load which falls on the injured muscle tissue and understand the limitations.
These sessions should help patients reach the edge of their limitations without over-exerting their injury. If a patient experiences a flare-up due to one of these sessions, they should relay this information to their therapist to adjust their training.
1. Massage and stretching
These tactics aim to extend and soften the injured muscle thereby decreasing the tension placed on it. Stretches will typically be done under the supervision of a trained professional as they can cause flare-ups if done improperly. If the emphasis of the stretch is placed on the back of the ankle, for example, the flexor hallucis longus tendon may become pinched and irritated.
Massages can be done at home, without supervision by using a foam roller, trigger ball, or a similar massage tool under the foot, at the back of the ankle, or on the calve. These simple tools can provide immediate relief at the onset of a flare-up and may alleviate pain completely for a small period.
2. Medication and pharmaceuticals
If the pain is persistent and robust, a doctor may prescribe medication or recommend over-the-counter anti-inflammatory medication. These medications can be used in conjunction with physical therapy or on their own to provide pain relief and reduce inflammation locally.
While these treatments can be an effective tool to help guide recovery, they do run the risk of addiction or even further degeneration of the tissue over prolonged use. A consultation from a medical expert is necessary before beginning a medication routine.
3. Splinting and load-bearing assistance
Splinting and the use of load-bearing devices such as canes are not typically required for flexor hallucis longus pain but can occasionally be recommended if the injury is severe enough. These devices help manage the physiology of movement around the flexor hallucis longus as well as decrease the load the injured muscle must bear.
4. Surgery
In the case of flexor hallucis longus discomfort, surgery is only used as a last option. When conservative treatment approaches fail, doctors may frequently propose more invasive surgery, which may include lengthy recovery periods, narcotic prescriptions, and aided rehabilitation before the muscle can be restored to function.
Even so, the flexor hallucis longus may never return to full function and may require a permanent routine of the above treatment methods post-surgery.
Regenerative Medicine and Flexor Hallucis Longus Pain
Conventional treatments may be sufficient to relieve the pain produced by flexor hallucis longus damage. But regenerative medicine can improve the body’s reaction to these therapies and give more long-term pain relief.
At CELLAXYS, we specialize in two forms of regenerative medicine – platelet-rich plasma therapy, or PRP, and cell-based therapies.
PRP therapy
In PRP, doctors first extract and isolate the platelets found in the blood and then reinject them into the injury site. Platelets naturally heal the body by binding to the damaged portions of tissue and then signaling the body to attract healing factors to their location.
They release 10 Growth Factors to stimulate the growth of healthy tissues and produce fibrin, a sticky web that serves as the scaffolding for new tissue development. A high amount of platelets in the injury site ensures speedy recovery and healing.
This therapy has been an effective treatment for several spine, orthopedic, and sports injuries. It is an outpatient procedure, so you can go right after the procedure, which takes about 45 minutes to complete.
Cell-based therapies
Also known as stem cell therapy, this treatment extracts healthy “autologous” tissues or cells from the patient’s body, processes them, and reinjects them to the injury site. Depending on your condition, the doctor may go for any of the two cell-based therapies:
- Minimally Manipulated Adipose Tissue (MMAT) transplant. This procedure is highly effective in many injuries. It involves harvesting cells from your adipose (fat) tissue and reinjecting them into the injury site. One great benefit of MMAT is that your doctor can perform it in multiple transplant locations in the same procedure.
- Bone Marrow Concentrate (BMAC). This procedure extracts highly concentrated cells from your bone marrow and reinjects them into the injury site.
Both cell-based therapies are performed under anesthesia, and the doctor uses live X-rays or ultrasound to detect the exact injury location. They take about 1.5 to 2 hours to complete and are outpatient procedures like PRP.
By using regenerative medicine alongside conventional forms of therapy, the recovery period for flexor hallucis longus injury can be cut substantially. PRP and cell-based therapies also provide long-lasting relief for about 6 months to a year.
Sources
Footnotes
- Schulhofer SD, Oloff LM. Flexor hallucis longus dysfunction: an overview. Clinics in podiatric medicine and surgery. 2002;19(3):411-8.
- Howard PD. Differential diagnosis of calf pain and weakness: flexor hallucis longus strain. Journal of Orthopaedic & Sports Physical Therapy. 2000;30(2):78-84.
- Oloff LM, Schulhofer SD. Flexor hallucis longus dysfunction. The Journal of foot and ankle surgery. 1998;37(2):101-9.
- Michelson J, Dunn L. Tenosynovitis of the flexor hallucis longus: a clinical study of the spectrum of presentation and treatment. Foot & ankle international. 2005;26(4):291-303.
- Rungprai C, Tennant JN, Phisitkul P. Disorders of the flexor hallucis longus and os trigonum. Clinics in Sports Medicine. 2015;34(4):741-59.
References
- Flexor hallucis longus. Physiopedia. Accessed 2/25/2024.
- Flexor Hallucis Longus Tendonitis. PhysioAdvisor. Accessed 2/25/2024.
- Flexor Hallucis Longus Tendonitis Symptoms & Treatment. Upswing Health. Accessed 2/25/2024.
- Tibial Nerve. Physiopedia. Accessed 2/25/2024.
CELLAXYS does not offer Stem Cell Therapy as a cure for any medical condition. No statements or treatments presented by Cellaxys have been evaluated or approved by the Food and Drug Administration (FDA). This site contains no medical advice. All statements and opinions are provided for educational and informational purposes only.
Dr Pejman Bady
Author
Dr. Pejman Bady began his career over 20 years ago in Family/Emergency Medicine, working in fast-paced emergency departments in Nevada and Kansas. He has served the people of Las Vegas as a physician for over two decades. Throughout this time, he has been met with much acclaim and is now the head of Emergency Medical Services in Nye County, Nevada. More about the doctor on this page.
Dr Pouya Mohajer
Contributor
Pouya Mohajer, M.D. is the Director of Spine and Interventional Medicine for CELLAXYS: Age, Regenerative, and Interventional Medicine Centers. He has over 20 years of experience in pain management, perioperative medicine, and anesthesiology. Dr. Mohajer founded and is the Medical Director of Southern Nevada Pain Specialists and PRIMMED Clinics. He has dedicated his career to surgical innovation and scientific advancement. More about the doctor on this page.









