Published on: November 26, 2019 | Updated on: November 4, 2024
Our knees are a crucial part of many physiological functions. One of the most important aspects of cushioning the knee is the meniscus, which acts as the “shock absorber.” The meniscus can be damaged in traumatic twisting events, but more commonly with time, as it begins to weaken with repetitive use. This can lead to pain and discomfort, typically on the knee’s inside (medial) or outside (lateral) joint line.
As a general rule, younger patients suffer from more trauma-induced injuries that tend to do better with surgery. Patients in their 30s and above tend to suffer from more micro-trauma-induced injuries that often can be treated without surgery.
A knee injury has the potential to derail many daily functions, from driving to walking. Once an injury disrupts daily life, consult a doctor to determine what is happening and how to resolve the issue.
Anatomy of the Knee
Inside the knee joint, there are a couple of significant structures: the femur, patella, femur, meniscus, and the stabilizing ligaments (ACL and PCL). The femur is the thigh bone, the patella is the kneecap, and the tibia is the shin bone.
The meniscus is two pieces of cartilage (“medial” and “lateral”) between the femur and tibia that cushion the bones during activity so that they don’t collide. Every joint in the body has a piece of cartilage between the bones. For this reason, they serve a vital role in the body’s ability to function.
Injury to the Meniscus
Due to its crucial location and shock-absorbing mechanism, the meniscus is prone to tearing. Individuals who participate in sports that quickly change direction, such as tennis or basketball, are at a higher risk.
Tears in the meniscus can begin as small and increase over time, or a significant tear can co-occur. There are six different types of meniscus tears:
- Radial Tear: A radial tear is the most common type of meniscus tear. Because this sort of tear develops in a part of the knee that isn’t supplied with blood, it won’t mend on its own. If the tear is significant, surgery may be necessary. The surgeon will trim away the injured section of the meniscus in the case of a radial tear.
- Horizontal Tear: One of the easiest tears to heal in the knee is a horizontal meniscus tear. Rather than removing the injured section of the meniscus, the surgeon will attempt to reattach the circumferential fibers of the meniscus. When it comes to meniscus repair, the location is crucial. The more vascular parts of the meniscus, along the outside border, have a higher chance of healing than those closer to the center of the knee.
- Intrasubstance/Incomplete Tear: On an MRI, physicians frequently observe partial meniscus tears in persons in their 20s and 30s. These tears are frequently indicative of early degenerative alterations in the meniscus. Meniscus tears that are just partially torn are called “stable” injuries. That is to say, they are usually not surgically treated.
- Flap Tear: A meniscus flap tear has a unique tear pattern. A piece of cartilage is ripped away and might become lodged in the joint, causing it to “catch” or lock up. If the flap causes the knee to catch, a surgeon can generally correct the problem without removing much tissue.
- Complex Tear: A complex tear has several tear patterns, including both radial and horizontal patterns. Because of its intricate nature, surgical repair is rarely used to treat it. In certain rare cases, a surgeon may be able to remove some of the torn menisci while mending the rest.
- Bucket-handle Tear: A bucket-handle tear is a common form of a horizontal meniscus tear. Because the torn component of the meniscus prevents normal knee mobility, these injuries frequently cause the knee to become stuck. Bucket-handle tears often need more immediate surgical intervention to allow the knee to flex again.
Causes
Many factors can cause a tear in the meniscus. The most common reason someone experiences a meniscus tear is because of an injury or repetitive micro-trauma.
These occur most often during sports or exercise, but depending on an individual’s overall health, they can also occur from a task as simple as walking around or a simple twisting motion.
A tear is more likely to occur if an individual is experiencing joint degeneration. Degeneration occurs when soft tissue is worn down over time and slowly becomes smaller. “Degenerative tears” most often begin to appear in patients above 40 years of age.
Conditions such as arthritis result from chronic, slowly evolving degeneration. When cartilage, both the meniscus and articular cartilage, can no longer protect bones, they begin to rub against one another, causing damage to the bone integrity and pain in the area.
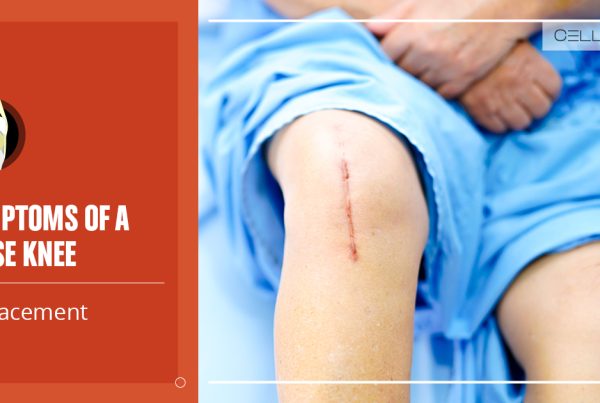
Signs and Symptoms
Tearing the meniscus can feel like a sharp pain or cause no initial sensation. Some individuals can hear or feel a “popping” sensation as the cartilage tears. It may not be readily apparent that a tear has occurred, but the knee typically becomes painful and swollen in the days following the injury.
Some individuals may continue to exercise without yet knowing that they have a tear. Common symptoms of a meniscus tear are:
- Pain in the knee
- Swelling
- Stiffness or inability to bend the knee
- Weakness or inability to put weight on the knee
Depending on the severity of the tear, symptoms can be chronic or only occur during certain activities. A doctor should be consulted once the symptoms begin to impact daily life.
Diagnosing a Meniscus Tear
Consulting with a doctor allows the recovery process to begin. During this meeting, they will ask about symptoms and family history; honesty is essential. Symptoms that may not seem relevant could be important indicators of what is causing pain.
They may observe how a patient walks, squats, or how far they can move their knee. Discussion and observation alone cannot often result in an accurate diagnosis, however, so doctors turn to proven diagnostic techniques to be sure of the cause:
- McMurray test: With the patient lying on their back, doctors bend the knee to indicate a meniscus tear. They listen for a popping or clicking sound, often indicative of a tear. This test is usually accurate if performed correctly, though some doctors prefer to use imaging techniques to be specific.
- MRI: Magnetic Resonance Imaging can create an image of a patient’s internal soft tissue. An MRI can detect most meniscus tears if there is a tear in the meniscus or any other soft tissue.
- X-ray: These are not often used for meniscus tears as they do not show soft tissue. However, they help determine bone abnormalities that could contribute to knee pain.
Multiple conditions can occur simultaneously. More than one diagnostic test can indicate all causes of knee pain. Knowing precisely what happens under the surface allows doctors to create an effective recovery plan that meets each patient’s needs.
Recovering From a Meniscus Tear
The recovery process will vary depending on the severity of the tear, where it is located, and how the tear is positioned among the cartilage and bone. Some minor tears do not require surgery, but in many cases, this injury leads to surgical intervention. Nonsurgical treatments may include:
- RICE Method: Rest, Ice, Compression, and Elevation. Resting the injury allows it to heal without added stress. Icing the knee can reduce inflammation, swelling, and pain. Compression prevents further damage and blood loss by reducing swelling. Elevating the injury can prevent blood clots and reduce swelling—the knee must be above the heart, which can be achieved by lying down and placing a pillow under the knee.
- Anti-Inflammatory Medication: Over-the-counter drugs such as ibuprofen or naproxen can reduce inflammation and pain.
- Physical Therapy: Physical therapy aims to restrengthen muscles, providing more support for the joint. The exercises in physical therapy can also improve blood flow, which sends the body’s healing properties to the injury and can lead to repair over time.
These treatments can potentially heal minor injuries but may not always work. Once these have been attempted with little to no pain relief, doctors will often turn to surgery to repair an injury. Sometimes, the injury is so severe that surgery is the first option.
Surgical Techniques for Meniscus Tear
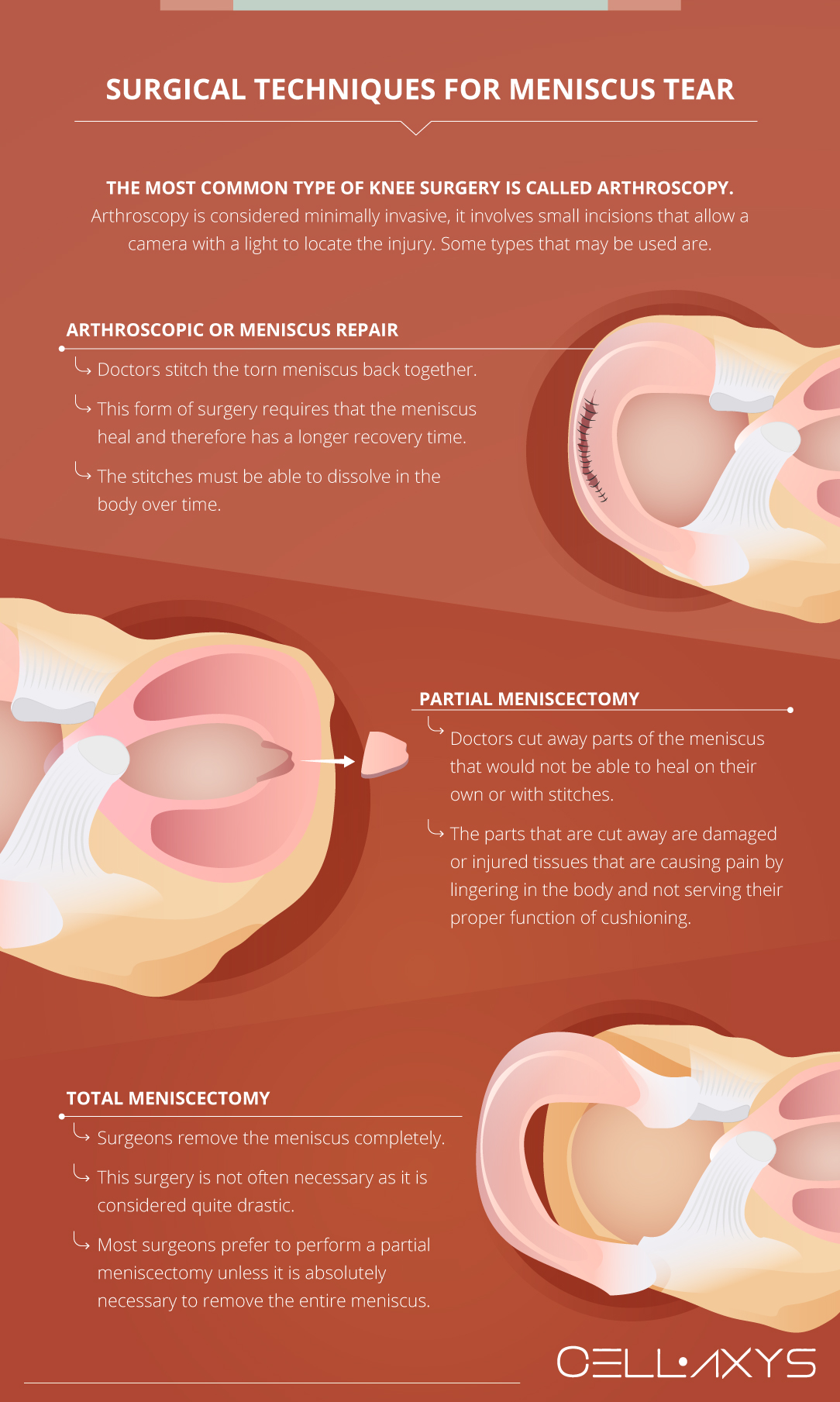
Several types of surgery may be done to repair a torn meniscus.
The most common type of knee surgery is called a partial meniscectomy, performed through arthroscopy. Arthroscopy is considered minimally invasive because it involves small incisions, allowing a light camera to locate the injury.
Once the injury has been found, surgeons enter the knee with the small tools that are necessary to make repairs. Types of arthroscopy that may be used are:
- Arthroscopic or Meniscus Repair: Only about 15% of Meniscus tears can be “repaired.” Doctors can attempt to repair the meniscus by stitching the torn meniscus back together. This form of surgery requires that the meniscus heal and, therefore, has a longer recovery time. It requires six weeks on crutches and is typically performed on younger patients.
- Partial Meniscectomy: By far, the most common meniscus surgery. Using an arthroscope, doctors can cut away or remove parts of the meniscus that would not be able to heal on their own or with stitches.
- Total Meniscectomy: This surgery is becoming increasingly rare because it causes early-onset arthritis. Although it is not often necessary, it is considered quite drastic, as it involves removing the entire portion of the meniscus.
Once the surgery is complete, doctors will set a recovery plan to ensure each patient can heal as quickly as possible. Postoperative plans often include the use of a walker, cane, crutches, or other assistive devices that reduce the amount of pressure on the knee and help with pain levels. Recovery involves physical therapy or exercises that ensure the knee heals properly.
The recovery time for knee surgery is typically short, 4-6 weeks. Most patients report decreased pain and the ability to walk within two weeks. In approximately two months, patients can begin to enjoy exercise again. This may vary depending on the severity of the injury and the patient’s commitment to the recovery process.
Though this recovery time is short relative to more invasive surgeries, some patients cannot afford to take so much time off of work. Before deciding to undergo surgery, it is important to consider all available options that may help heal the injury.
Alternatives to Surgery for Meniscus Tears
Doctors will use surgical and nonsurgical approaches to treat meniscus tears, depending on the severity of the problem and the patient’s health conditions. Surgery is not recommended for low-grade pain and minimal tearing. Certain alternatives can help manage the pain and heal the tear.
Physical Therapy
Physical therapy is recommended to strengthen the muscles around the knee. It helps in regaining flexibility and also makes the joint more stable. Specific exercises will strengthen the quadriceps, hamstrings, and calf muscles.
When the muscles get strong, they exert minimal pressure on the knee, making it easy to move it around.
The good thing about physical therapy is it is non-invasive and can manage pain and swelling quickly without any intervention.
Corticosteroid Injections
These anti-inflammatory drugs are injected directly into the knee to alleviate pain and swelling. The treatment provides temporary relief by reducing the inflammation. Although it doesn’t help heal the tear, it is good for short-term pain management.
Comparing Surgical and Non-surgical Options
Alternative treatments may provide temporary relief, but surgery may sometimes be unavoidable.
Here is a comparison of both options to understand when it’s best to wait it out and when you can’t delay the surgery.
Surgery
Two of the primary surgical options available to you are arthroscopic meniscus repair surgery and partial meniscectomy.
Arthroscopic meniscus repair surgery attempts to recover the knee completely. It is recommended for major tears. However, the downside is that recovery lasts 6 to 7 months.
This surgery is recommended for young individuals with an active lifestyle and no underlying health conditions.
Partial meniscectomy, on the other hand, has a short recovery time and is done to remove the damaged part of the meniscus only. However, this surgery may lead to osteoarthritis, as much of the cartilage cushioning is lost during surgery.
This surgery is recommended for people with irreparable tears or tears in the avascular zones.
Non-Surgical Options
Nonsurgical options are noninvasive, of course, and prevent the need for surgery.
Although these are not recommended when tearing is severe, physical therapy, PRP stem cell therapies, and corticosteroid injections are available. All of these manage pain and promote tissue regeneration and healing.
Let’s check out some cell-based therapy options we have today.
Regenerative Therapies
The burgeoning field of Regenerative Medicine and Cell-Based Procedures offers new hope to patients suffering from meniscus tears. These therapies work particularly well on soft tissue, which gives them an advantage in repairing this specific injury. There are two types of regenerative therapy offered at CELLAXYS:
Autologous Stem Cell Procedures
Autologous stem cell procedures begin with taking cells from a patient’s adipose (fat) tissue, blood cells, or bone marrow. These cells are then processed to be concentrated and reinjected into the injury site. These cells contain healing properties that the body uses naturally to repair minor damages. Increasing the concentration of these cells could lead to a faster recovery.
Cell-based therapy or Autologous Stem Cell Procedures begin with an extract of stem cell-rich adipose (fat) tissue or bone marrow. This tissue is then minimally manipulated and prepared to be transplanted into the knee. The transplantation will be performed under live X-ray, called fluoroscopy, and Ultrasound together while you are under anesthesia.
Stem cell-rich tissues stimulate and re-initiate the body’s natural healing process. At Cellaxys, a specific procedure called Minimally Manipulated Adipose Tissue Transplant tends to be the most requested procedure for meniscus tears in patients over 40 and bone marrow-derived stem cells in patients under 40.
Treatments like these are essential to consider when faced with all of the options, as they are some of the only treatments on the market that seek to address and correct the actual cause of injury rather than just manage symptoms.
Cell-based medicine can be a good option to prevent the need for surgery in many patients. It can also be used after an operation to help repair damaged tissue, specifically in patients suffering from pain after meniscus surgery.
Clinical studies have demonstrated thicker, stronger-appearing meniscus one year after the procedure. This has been demonstrated using both adipose and bone marrow-derived stem cells.
Platelet-Rich Plasma (PRP) Therapy
This form of therapy begins with a simple blood draw. The patient’s blood is then placed in a centrifuge to isolate the platelets from other components in the blood. Once the solution is processed, it is injected into the injury site. Platelets contain proteins and healing factors, namely ten different growth factors, that the body uses to repair damaged tissue. Undergoing PRP can allow an injury or tear to heal more quickly with more healing properties.
All Cell-Based procedures are performed as outpatient procedures. The recovery time is much shorter than surgery. Patients who receive these procedures commonly return to normal activities within a few days.
Depending on the severity of the tear, meniscus tear injuries may require surgical intervention. In these cases, Cell-Based procedures can be used as an adjunct to surgery as a sort of “boost” to help the injury heal post-op. In many cases, regenerative Cell-Based procedures improve pain and function to the point where surgery is no longer necessary.
Sources
Footnotes
- Doral MN, Bilge O, Huri G, Turhan E, Verdonk R. Modern treatment of meniscal tears. EFORT open reviews. 2018;3(5):260-8.
- Mordecai SC, Al-Hadithy N, Ware HE, Gupte CM. Treatment of meniscal tears: an evidence based approach. World journal of orthopedics. 2014;5(3):233.
- Cengiz IF, Pereira H, Espregueira-Mendes J, Oliveira JM, Reis RL. Treatments of meniscus lesions of the knee: current concepts and future perspectives. Regenerative Engineering and Translational Medicine. 2017;3:32-50.
- Howell R, Kumar NS, Patel N, Tom J. Degenerative meniscus: Pathogenesis, diagnosis, and treatment options. World journal of orthopedics. 2014;5(5):597.
- Thorlund JB, Juhl CB, Ingelsrud LH, Skou ST. Risk factors, diagnosis and non-surgical treatment for meniscal tears: evidence and recommendations: a statement paper commissioned by the Danish Society of Sports Physical Therapy (DSSF). British Journal of Sports Medicine. 2018 May 1;52(9):557-65.
References
- Nonsurgical Treatments for Meniscus Tears. NYU Langone Hospitals. Accessed 2/23/2024.
- Torn meniscus. Mayo Clinic. Accessed 2/23/2024.
- Meniscus Tears: Symptoms, Diagnosis, and Treatment. Verywell Health. Accessed 2/23/2024.
- Knee Anatomy. ARTHRITIS-Health. Accessed 2/23/2024.
- Arthritis. Mayo Clinic. Accessed 2/23/2024.
CELLAXYS does not offer Stem Cell Therapy as a cure for any medical condition. No statements or treatments presented by Cellaxys have been evaluated or approved by the Food and Drug Administration (FDA). This site contains no medical advice. All statements and opinions are provided for educational and informational purposes only.
Dr Pejman Bady
Author
Dr. Pejman Bady began his career over 20 years ago in Family/Emergency Medicine, working in fast-paced emergency departments in Nevada and Kansas. He has served the people of Las Vegas as a physician for over two decades. Throughout this time, he has been met with much acclaim and is now the head of Emergency Medical Services in Nye County, Nevada. More about the doctor on this page.
Dr Pouya Mohajer
Contributor
Pouya Mohajer, M.D. is the Director of Spine and Interventional Medicine for CELLAXYS: Age, Regenerative, and Interventional Medicine Centers. He has over 20 years of experience in pain management, perioperative medicine, and anesthesiology. Dr. Mohajer founded and is the Medical Director of Southern Nevada Pain Specialists and PRIMMED Clinics. He has dedicated his career to surgical innovation and scientific advancement. More about the doctor on this page.