Published on: February 26, 2020 | Updated on: August 29, 2024
Table of contents
- Intro
- What Causes Pinched Nerves In the Spine?
- What Are Cervical Epidural Steroid Injections?
- How Do Cervical Epidural Steroid Injections Work?
- How Successful Are Cervical Epidural Steroid Injections?
- What Are the Risks of Cervical Epidural Steroid Injections?
- Infection
- Spinal Cord, Brain, and Nerve Injury
- Weakened Bone and Muscle Structures
- What Alternatives Exist for Nerve-Related Pain?
- Regenerative Medicine and Nerve Pain
Cervical epidural steroid injections are treatments intended to relieve pain in the upper body and arms caused by pinched or inflamed nerves in the cervical spine. This type of injury can have a drastic impact on a person’s quality of life, especially as the structures of the spine degenerate.
Although steroidal injections have been demonstrated to be effective in the treatment of nerve pain, the treatment techniques, success rates, and hazards vary so widely that patients should do their homework before undergoing such procedures.
What Causes Pinched Nerves In the Spine?
Often referred to as cervical radiculopathy, pinched nerves in the cervical spine may occur due to several inciting factors. Chronic illnesses such as arthritis and spinal stenosis, acute injuries, and “wear and tear” issues such as disc herniation can all lead to some level of cervical radiculopathy.
As the issues intensify, the structural integrity of the cervical spine begins to collapse, putting undue pressure on the nerves in the neck. Unfortunately, nerves do not respond well to the added stress and eventually, the pressure on the pinched nerves causes inflammation and pain which radiates throughout the upper back and along the arms. These issues can also be accompanied by muscle weakness, numbness, and a limited range of motion.
Though these issues may cause quite a disruption in a person’s daily life, cervical radiculopathy tends to respond well to conservative treatments. One of the most popular of these conservative treatments is a procedure known as a cervical epidural steroid injection.
What Are Cervical Epidural Steroid Injections?
An injection of steroids in the epidural space of the cervical spine is known as a cervical epidural steroid injection. By reducing the inflammatory levels of the pinched nerves, these injections attempt to help control the discomfort produced by cervical radiculopathy.
Corticosteroids often referred to simply as steroids contain the active ingredient in many steroidal injection therapies, including cervical epidural steroid injections. These steroids are lab-developed drugs made to closely resemble cortisol – a hormone the body naturally produces to help respond to stress.
While there are many types of corticosteroids (cortisone, prednisone, and methylprednisolone), the most commonly used in instances of cervical radiculopathy is dexamethasone.
Cervical epidural steroid injections are typically outpatient procedures, taking less than 15 minutes to administer. Initial side effects are mild and may take 2-3 days to clear before the drugs take effect. Patients often report relief lasting anywhere from 2 weeks to several months.
Cervical epidural steroid injections, just like most steroidal treatments, must be administered periodically as symptoms manifest in patients. Though initial side effects are mild, prolonged use of steroids can have several adverse consequences. As a result, many medical professionals recommend limiting the total number of injections to 3 to 4 per year.
How Do Cervical Epidural Steroid Injections Work?
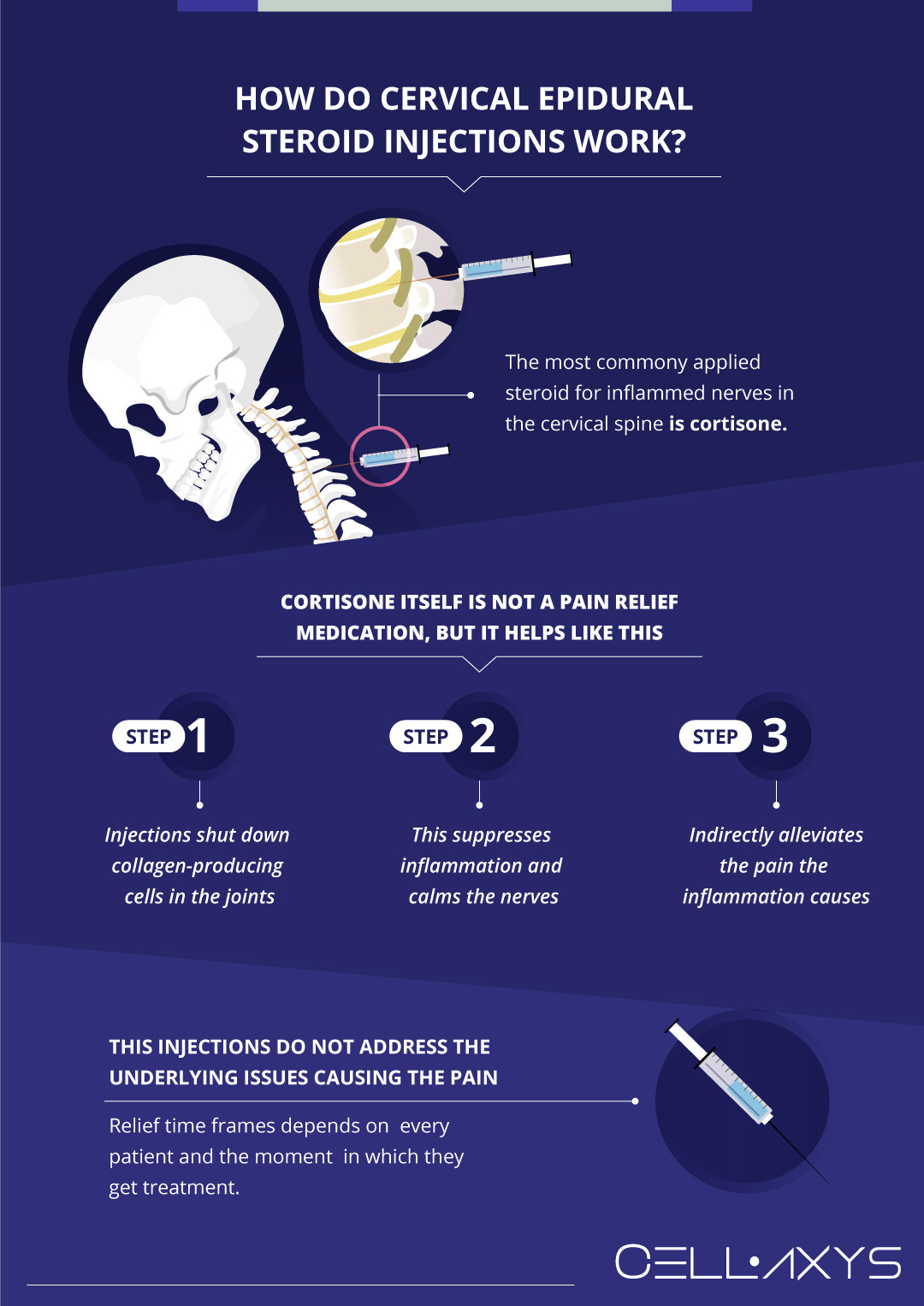
Dexamethasone is not a pain reliever, even if it is used to alleviate the pain produced by pinched nerves. Instead, dexamethasone actively works to reduce inflammation and indirectly alleviate the pain this inflammation causes. Therefore, the injections do not address the underlying issues causing the pain, but instead, treat one of the symptoms these issues create.
Because patients may pursue this treatment at different points in the development of their pinched nerve, the relief due to cervical epidural steroid injections can have different time frames for each person.
Some patients report immediate relief, while for others, relief may take some time. If the cervical radiculopathy is severe or if it is due to a chronic issue, relief may not be adequate or may never come.
How Successful Are Cervical Epidural Steroid Injections?
Success rates for cervical epidural steroid injections are largely subjective, though what most patients consider success is pain relief and management. Several studies have been conducted to quantify the efficacy of these treatments, with varying results.
One study by the Journal of Spinal Disorders and Techniques in 2006, followed 70 patients through their cervical epidural steroid procedure. Of these 70 patients, 44 (63%) found prolonged relief from their cervical radiculopathy, enough to reconsider surgical intervention.
In another study conducted for the Humana Press, only 38% of those treated found any relief whatsoever after administering cervical epidural steroid injections for their pain.
The FDA has released several statements disparaging the efficacy of steroidal injections for pain management, citing their use as a major causal factor for “serious neurologic adverse events.”
Though steroidal injections may provide pain relief for certain patients, the majority of evidence suggests that long-term usage of these medications might lead to greater problems in any patient who receives them.
What Are the Risks of Cervical Epidural Steroid Injections?
As with any medicine, risks exist when applying cervical epidural steroid injections. While doctors and clinical specialists can offer some guidance, it is ultimately up to the patient to decide if these risks outweigh the benefits when choosing to apply steroids to their issue.
Some of the more rare but severe side-effects of cervical epidural steroid injections include:
- Infection
- Spinal cord, brain, and nerve injury
- Weakened bone and muscle structures
Less severe, but more likely reactions include:
- Insomnia
- High blood sugar
Infection
Infection due to steroid injection is fairly uncommon, though not completely absent. In an article posted by the Center for Disease Control in 2012, the organization discovered an outbreak of a deadly strain of meningitis that traced back to three lots of contaminated steroid solutions made in Massachusetts.
A month after the article was posted, the FDA had identified 137 cases of the outbreak with 12 confirmed deaths in 10 states due to the bad batch of steroids.
Furthermore, a study by Deutsches Ärzteblatt International, the official journal of the German Medical Association and the National Association of Statutory Health Insurance Physicians, found that “repeated injections with too little time between them raise the risk of infection.”
In the study, DA International found that of 1528 cases examined, 223 (15%) were found to have suffered an infection tracing back to their use of steroid injection.
Spinal Cord, Brain, and Nerve Injury
In a study of claims filed by 35 US liability insurance companies published by Anesthesiology, the journal found that some of the most common claim-related incidents involved “direct needle trauma to a nerve or the spinal cord” and “cord infarction/stroke after the intra-arterial injection”. Together, these incidents accounted for 45% of insurance claims involved in cervical procedures.
Weakened Bone and Muscle Structures
One of the most studied and generally accepted risks of repeated steroid use is weakened bone and muscle structure.
Studies have indicated that bone mineral density decreases with repeated steroid use and that these treatments significantly increase the chances of a person developing osteoporosis and osteopenia. These weakened bone structures were also linked to an increased risk of bone fracture according to one scientific journal.
What Alternatives Exist for Nerve-Related Pain?
Cervical epidural steroid injections are a prevalent therapy in the United States, however, the hazards associated with them may deter potential patients from undergoing such procedures. Furthermore, for some individuals, even conservative treatment choices (physical therapy and over-the-counter medicine) may not be enough to relieve irritated or pinched nerves.
While surgery may appear to be the only option for a patient, new advances in the field of regenerative medicine suggest that this is not the case.
Regenerative Medicine and Nerve Pain
While steroid injections may relieve the pain caused by inflamed and pinched nerves, the underlying issue persists and may get worse over time due to the characteristics of steroids. Regenerative therapies offer a solution to these problems by treating both the symptoms of inflamed nerves and their inciting factors.
Furthermore, because the source materials come directly from the patients and are administered using state-of-the-art technologies, mesenchymal stem cells and platelet-rich plasma (PRP) injections, such as those offered at Cellaxys, reduce some of the potential risks associated with steroid injections.
The platelet-rich plasma, derived from the patient’s own blood, is a mixture of the plasma found in the blood and natural growth factors. Mesenchymal stem cells are obtained from the bone marrow.
After harvesting and processing cells from blood and bone marrow, directly from the patient, they are then injected into the area of pain. The doctors at Cellaxys can create treatments that induce and amplify the body’s own healing responses.
Our physicians can guarantee that these treatments reach the areas where they will be most helpful by injecting them using a live X-ray (fluoroscopy) guided injection.
Much like steroid injections, once inside the body, these treatments reduce inflammation by sending out chemical impulses that dull the body’s natural response to stress. However, unlike steroids, these injections do not limit the body’s healing responses, and thus do not deplete the resources necessary to keep the bone and muscle structures intact.
Sources
Footnotes
- Kim S, Hwang B. Relationship between bone mineral density and the frequent administration of epidural steroid injections in postmenopausal women with low back pain. Pain Research and Management. 2014;19:30-4.
- Kerezoudis P, Rinaldo L, Alvi MA, Hunt CL, Qu W, Maus TP, Bydon M. The effect of epidural steroid injections on bone mineral density and vertebral fracture risk: a systematic review and critical appraisal of current literature. Pain Medicine. 2018;19(3):569-79.
- Lin EL, Lieu V, Halevi L, Shamie AN, Wang JC. Cervical epidural steroid injections for symptomatic disc herniations. Clinical Spine Surgery. 2006;19(3):183-6.
- Huston CW. Cervical epidural steroid injections in the management of cervical radiculitis: interlaminar versus transforaminal. A review. Current Reviews in Musculoskeletal Medicine. 2009;2:30-42.
- Cicala RS, Westbrook L, Angel JJ. Side effects and complications of cervical epidural steroid injections. Journal of pain and symptom management. 1989;4(2):64-6.
- Centers for Disease Control and Prevention (CDC). Multistate outbreak of fungal infection associated with injection of methylprednisolone acetate solution from a single compounding pharmacy-United States, 2012. MMWR. Morbidity and mortality weekly report. 2012;61(41):839-42.
- Holland C, Jaeger L, Smentkowski U, Weber B, Otto C. Septic and aseptic complications of corticosteroid injections: an assessment of 278 cases reviewed by expert commissions and mediation boards from 2005 to 2009. Deutsches Ärzteblatt international. 2012;109(24):425.
References
- Cervical Radiculopathy: Non-operative Treatments and Cervical Epidural Steroid Injection. HSS. Accessed 2/23/2024.
- Dexamethason. Medline Plus. Accessed 2/23/2024.
- Cortisol. You & Your Hormones. Accessed 2/23/2024.
- Cortisone shots. Mayo Clinic. Accessed 2/23/2024.
- FDA Drug Safety Communication: FDA requires label changes to warn of rare but serious neurologic problems after epidural corticosteroid injections for pain. FDA. Accessed 2/23/2024.
CELLAXYS does not offer Stem Cell Therapy as a cure for any medical condition. No statements or treatments presented by Cellaxys have been evaluated or approved by the Food and Drug Administration (FDA). This site contains no medical advice. All statements and opinions are provided for educational and informational purposes only.
Dr Pouya Mohajer
Author
Pouya Mohajer, M.D. is the Director of Spine and Interventional Medicine for CELLAXYS: Age, Regenerative, and Interventional Medicine Centers. He has over 20 years of experience in pain management, perioperative medicine, and anesthesiology. Dr. Mohajer founded and is the Medical Director of Southern Nevada Pain Specialists and PRIMMED Clinics. He has dedicated his career to surgical innovation and scientific advancement. More about the doctor on this page.
Dr Pejman Bady
Contributor
Dr. Pejman Bady began his career over 20 years ago in Family/Emergency Medicine, working in fast-paced emergency departments in Nevada and Kansas. He has served the people of Las Vegas as a physician for over two decades. Throughout this time, he has been met with much acclaim and is now the head of Emergency Medical Services in Nye County, Nevada. More about the doctor on this page.