Published on: January 27, 2020 | Updated on: August 29, 2024
Though muscle strain is one of the most common athletic injuries, it can happen to anyone at any time. A calf strain can cause pain and prevent you from running, jumping and doing other activities. A severely pulled calf muscle can result in partial or complete tears.
The tear can vary in size and may have different symptoms depending on the severity. A torn calf muscle may require treatments such as surgery or alternative therapies such as regenerative medicine.
Do you have calf strains?
Fill out the form below to schedule your FREE virtual consultation
Anatomy of the Calf
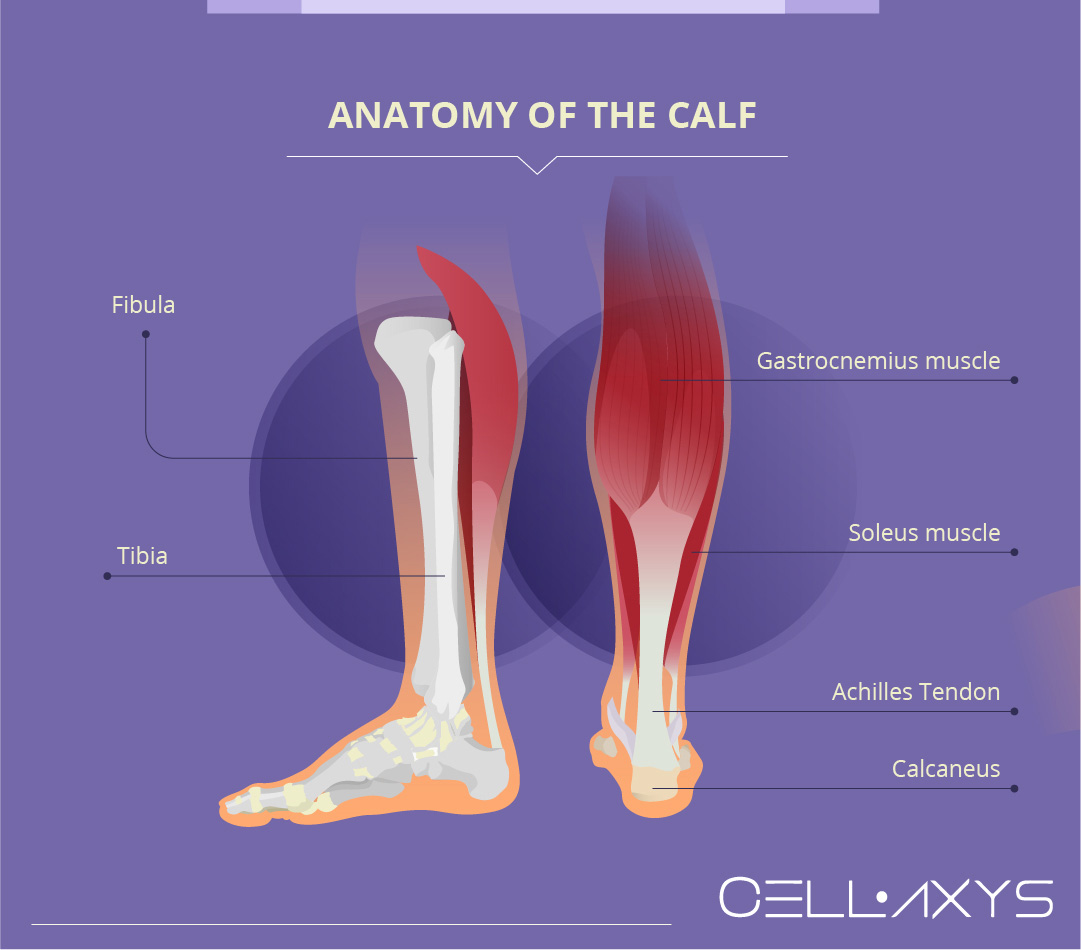
The calf is composed of bones, muscles, and tendons that work together to keep it functional and stable. The major muscle of the calf is called the gastrocnemius. This muscle is located in the top half of the calf and is sometimes visible from the outside.
The soleus muscle is under the gastrocnemius and under the Achilles tendon. The soleus muscle enables our ability to walk, run, and dance. It is also a major postural muscle designed to stop the body from falling forwards at the ankle during stance.
Major bones in the calf are the tibia and fibula. These work together with the calcaneus in the ankle to allow for support and stability in the calf.
The Achilles tendon connects the calf muscles to the calcaneus. This tendon is a crucial part of all motion involving the leg, foot, and ankle. Damage to the Achilles tendon can cause severe instability and pain, and if left untreated can lead to significant issues later in life.
A strain to the muscle is different from a sprain. Sprains are characterized by damage to ligaments, which connect bone to bone. This can be in the form of a tear or simply overstretched muscle. Sprains can influence the stability of a joint by loosening the connection between two major parts of it.
Strains are characterized by damage to muscle or tendons. These soft tissues may be torn or overstretched. A strain can occur as a result of misuse or overuse. Repetitive motions are a common reason why strains occur, though they may occur due to being bent or overexerted. Some individuals have muscle strain after using the muscles in an unfamiliar way during exercise or other activity. Strains are also sometimes referred to as a “pulled” muscle.
Diagnosing Calf Strain
It is rather easy to notice a calf strain if you know what to look for. There are several symptoms, including:
- Pain during activity or motion
- Bruising
- Swelling
- Tenderness
- Tearing sensation
A strain on the gastrocnemius might result in acute pain, a subtle discomfort, or something in between. The discomfort is usually felt at the back of the lower leg, although it can also affect the foot. Many people who have had a calf strain have difficulty walking because of discomfort or a loss of stability.
If you suspect a strain, you should consult a doctor right away. Injuries are more likely to heal incorrectly if they are not treated by a medical practitioner. Improper healing can lead to issues with the soft tissue later in life.
The process of diagnosing a calf strain begins with a consultation. Doctors will inquire about your medical history, past injuries, amount of exercise, and the cause of your calf injury. They will pay attention to the symptoms and examine the region for pain, bruising, and swelling. They could watch the patient walk or do other activities to figure out where the injury came from.
There are three major classifications of calf strain:
- Grade 1: sometimes referred to as a “mild” injury, a grade 1 calf strain is a minor tear in the muscle. This is the most common form of a calf strain and many individuals who experience it can still walk or move around. It typically takes 1-3 weeks to fully heal.
- Grade 2: sometimes referred to as a “moderate” injury, grade 2 calf strains are also the result of a tear to the muscle. Though a grade 2 injury is more severe, it is not a complete tear. Individuals who have experienced this level of tear should expect to recover within 3-6 weeks.
- Grade 3: sometimes referred to as a “severe injury”, a grade 3 calf strain is a full tear of the muscle. Grade 3 calf strains should be immediately addressed by a doctor and often require surgery to correct. Due to the severity of the injury, it can take 6 months to a year to fully heal. Severe calf strains may cause a hematoma and should be examined by a medical professional immediately.
Many doctors use an imaging technique like an Ultrasound to determine the extent of damage, though they may also use MRI or CT Scans. These allow doctors to gather a picture of the soft tissue and assess the severity of the injury. Knowing exactly what is happening inside the body can inform surgical decisions and treatment. X-rays are not often used as they only show bone and calf strains are an injury to soft tissue.
Conventional Treatments for Calf Strain
Each individual patient will experience a different recovery process. Techniques that work for one person may not work for everyone. Doctors will encourage patients to try different treatments to see what is best for them.
Determining the most effective treatment will also depend on the severity of the injury. For minor injuries, resting the muscle is often enough for it to heal completely. As the injury becomes more severe, the treatment becomes more aggressive. Some of the most common treatments for calf strain are:
- RICE method: minor and moderate injuries respond well to the RICE method. RICE stands for Rest, Ice, Compression, and Elevation. Rest allows the muscles to heal, while ice and elevation help with swelling. Compression can help with swelling as well as prevent blood clots.
- Anti-inflammatory drugs: over-the-counter drugs such as Ibuprofen or Naproxen can help reduce swelling and ease pain associated with the injury.
- Corticosteroid injections: some doctors will suggest steroid injections, which deliver a powerful anti-inflammatory hormone to the injury site. These can cause long-term damage to soft tissue over time, so they should be closely monitored.
- Physical therapy/exercise: some patients respond well to certain exercises. Unlike some other injuries, exercise should not be used until the injury has had time to rest and heal. The goals of physical therapy are to improve strength, function, and stability. Certain exercises are not recommended as they can injure the muscle further, so consult a therapist before trying any exercises.
- Surgery: most calf strains will not require surgery, but when the muscle ruptures completely it becomes necessary to reattach the muscles. The recovery process for this surgery often lasts from 6 months to a year. Knowing what to expect before, during, and after surgery can be extremely beneficial to a patient. Being aware of what exactly is going to happen and the potential risks can greatly ease any anxiety or stress that comes with making the decision.
Results from treatment will vary for every patient. Certain treatments may be delayed until the injury is healed a certain amount, or avoided altogether if it’s not beneficial to the patient.
Calf Strain Recovery Timeline
Though each individual’s timeline is unique, there is a general pattern that can be expected if further complications do not occur. Causing the injury to become worse or more torn can lead to a slower recovery process.
Certain behaviors or conditions can make the recovery process take longer, such as diabetes, age, and smoking status. This timeline is a general guide to calf strain recovery and may not reflect your experience exactly.
The recovery timeline for most patients is as follows:
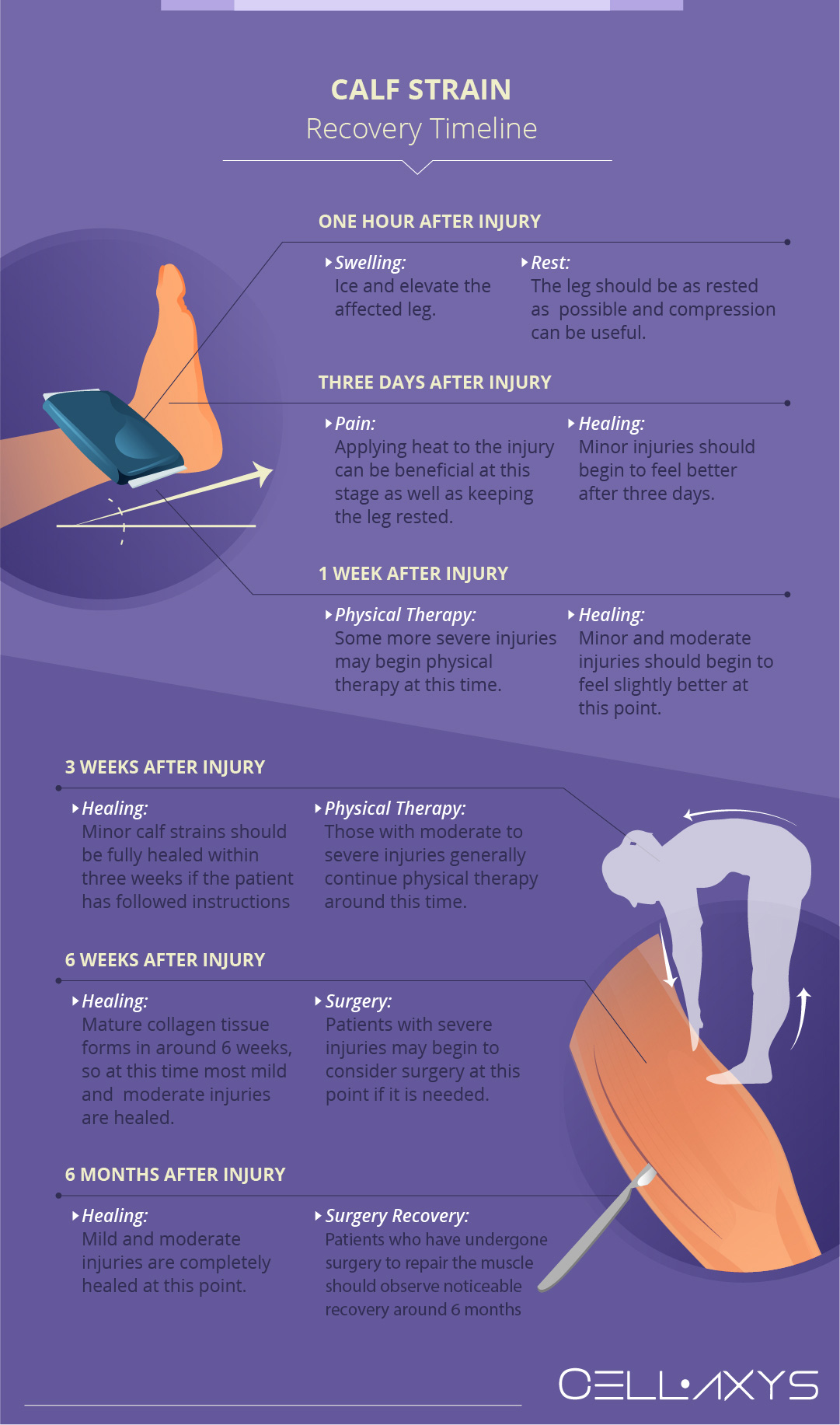
- One hour after injury: ice and elevate the affected leg to reduce swelling. Compression can also be beneficial at this stage. Do not apply heat as it can contribute to swelling. The leg should be as rested as possible. If mobility is hindered, make an appointment with a doctor to examine the injured calf.
- Three days after injury: applying heat to the injury can be beneficial at this stage as a form of pain relief. The injury should continue to remain as rested as possible. Minor injuries should begin to feel better after 3 days.
- One week after injury: minor and moderate injuries should begin to feel slightly better at this point with the proper amount of rest. Some more severe injuries may begin physical therapy at this time, though in the beginning it is limited to avoid further damage to the muscle tissue.
- Three weeks after injury: minor calf strains should be fully healed within 3 weeks if the patient has followed instructions. Patients whose injuries have healed can return to activities as normal. Those with moderate to severe injuries generally continue physical therapy around this time.
- 6 weeks after injury: mature collagen tissue forms in around 6 weeks, so at this time most mild and moderate injuries are healed. Patients can return to normal activities with a doctor’s approval. Patients with severe injuries may begin to consider surgery at this point, as it will be apparent if their injury is not healing through non-invasive treatment.
- 6 months after injury: mild and moderate injuries are completely healed at this point. Patients who have undergone surgery to repair the muscle should observe noticeable recovery around 6 months. By one year, all types of injury should be back to activity with minimal pain and discomfort.
The Role of Regenerative Medicine in Calf Strain Recovery
Significant progress has been made recently in the field of regenerative medicine. Soft tissue injuries in particular have taken well to this new form of therapy. Using stem cells or platelet-rich plasma, these types of therapy offer pain relief and faster healing for patients suffering from an injury to the calf muscle.
In some cases, it can even allow patients to surpass the need for surgery. CELLAXYS offers two types of regenerative therapy:
- Autologous stem cell therapy: this form of therapy begins with taking a patient’s stem cells, which are harvested using blood cells, fat cells, or bone marrow. The cells are processed to be more concentrated, then reinjected into the calf muscle. Stem cells contain healing properties that the body already sends to an injury, which can aid in collagen production – allowing scars to heal and the wound to close. Placing a concentrated stem cell solution into a part of the body that is healing can help the damage heal faster.
- Platelet-rich plasma therapy: this form of therapy begins with a simple blood draw. The patient’s blood is then placed in a centrifuge to separate platelets from other components in the blood. The platelets are then injected into the injury or surgery site. Platelets contain proteins and growth factors that the body uses naturally to heal damage. Increasing the number of platelets at the site of a tear could help it heal more quickly and stronger.
Both types of regenerative therapy have a low risk of rejection, as they are able to use a patient’s own cells. Some pain at the injection site may occur but typically is relieved in a matter of days.
Regenerative therapy can be used for mild, moderate, and severe injuries. It can be used to help an injury heal before or after surgery, and allow patients to participate more in physical therapy and early activities.
Some patients have been able to heal to the point where they no longer need surgery. When this is the case, the recovery process is simplified drastically.
CELLAXYS does not offer Stem Cell Therapy as a cure for any medical condition. No statements or treatments presented by Cellaxys have been evaluated or approved by the Food and Drug Administration (FDA). This site contains no medical advice. All statements and opinions are provided for educational and informational purposes only.
Dr Pejman Bady
Author
Dr. Pejman Bady began his career over 20 years ago in Family/Emergency Medicine, working in fast-paced emergency departments in Nevada and Kansas. He has served the people of Las Vegas as a physician for over two decades. Throughout this time, he has been met with much acclaim and is now the head of Emergency Medical Services in Nye County, Nevada. More about the doctor on this page.
Dr Pouya Mohajer
Contributor
Pouya Mohajer, M.D. is the Director of Spine and Interventional Medicine for CELLAXYS: Age, Regenerative, and Interventional Medicine Centers. He has over 20 years of experience in pain management, perioperative medicine, and anesthesiology. Dr. Mohajer founded and is the Medical Director of Southern Nevada Pain Specialists and PRIMMED Clinics. He has dedicated his career to surgical innovation and scientific advancement. More about the doctor on this page.









